Last Updated on November 11, 2019 by Heather Hart, ACSM EP, CSCS
Forewarning: there are semi graphic pictures in this post of my umbilical hernia surgery recovery and incision.
Disclaimer: the following are suggestions based on my experience with umbilical hernia surgery recovery. Always follow the advice of your doctor, and consult with your doctor if you have any questions or concerns.
I toyed with writing this piece like a race recap, because in all honesty, this experience has felt like a really long race. There were highs (some natural, some drug induced), there were lows, and there were points where my nutrition totally affected my performance, if you will. I bonked, I came back around, and now I think I can see the finish line. Alas, due to the wonderful power of search engines, I realize many non runners will show up to this very post looking for a little umbilical hernia surgery reassurance before their own procedure, so I’ll keep it simple, and leave out technical terms like “FOMO” and the aforementioned “bonk“. At least for now.
Instead I thought it would be helpful to write a list of tips learned through trial and error over the course of 11 days (and counting) of my umbilical hernia surgery recovery. Prior to surgery I reached out to the wonderful world wide web looking for first hand experiences and suggestions, and came up with a lot of generic medical posts instead. While semi helpful, they didn’t give me as much insight as I would have hoped. Over 500,000 hernia repairs occur per year in our country (source); with such a high occurrence rate, I was surprised to not find more personal experiences. Finding a firsthand experience from a fellow runner/athlete was near impossible. So here I am, oversharing with the world once again, in hopes that it might help someone.
What to Expect During Umbilical Hernia Surgery Recovery
Real talk: this surgery knocked me off my feet for a lot longer than I anticipated, a lot longer than my surgeon initially led me to believe. Yet, it didn’t leave me out of commission nearly as long as many friends and online acquaintances experienced. Thus, what I’m about to share was simply MY experience, and will obviously differ based on numerous factors surrounding your own procedure, body, prior training and racing experience…oh wait, scratch that last one.
Parameters surrounding my surgery:
What: An umbilical hernia that made it’s way through a small diastasis (about two fingers, moms reading this know that this is how diastasis recti is typically measured.)
Who: Me (obviously). 32 years old. For the moms checking in, 6 years post partum with two children. For what it’s worth (because I believe it has had a huge impact on my recovery), I am highy active: strength training 5 days per week and running approximately 25 +/- miles per week prior to surgery. I work as a personal trainer, so having the hernia fixed was essential.
Procedure: Umbilical herniorrhaphy with mesh. Non laparoscopic (traditional incision). Diastasis was left untouched.
(To catch you up on the pre-op and first 72 hours post surgery, much of which was rambling and written under the influence of the prescribed pain killers, read this post.)
1) This was a bigger deal than expected.
Other than a wisdom teeth extraction, I’ve never had surgery. Thus I’ll admit I went into this procedure pretty oblivious to what to expect post surgery. Initially, my surgeon told me “48 hours of pain, then you’ll be up and about. 2 weeks until you return to normal activity.” I took his word for it. In actuality, the pain lasted for about 5-6 days, discomfort for the next few days. I’m now 11 days post op and feeling 90% back to normal, though I have not yet resumed normal activity (i.e., working out). But during that first week, I was surprised at how incapacitated I was (more on this later). At my post op checkup (day #8), my surgeon explained to me that in the past, they would typically keep hernia surgery patients in the hospital for a day or two, then restrict them from normal activity for 6 weeks. He reminded me that while they’ve come a long way with this particular procedure, it is indeed still surgery, and nothing to be taken lightly.
2) You’re likely going to swell.
I felt, and looked, about 4 months pregnant for nearly the first week after surgery. This is natural, as with anything “traumatic” that occurs to your body; swelling is your body’s natural inflammatory response to any injury. Cells are dying, fluids are rushing to the area to aid in healing, but the fluid isn’t being removed as quickly as normal. So:
- Break out your most comfortable, loose fitting clothing. Sweatpants, yoga pants, you get the idea.
- ICE. Ice helps reduce swelling, and also helps ease some of the pain. I found a cold gel pack
to be the best option, because it not only conformed to the shape of my stomach, but it wasn’t quite as painfully cold as straight ice. Therefore the few times I fell asleep with it on (not recommended!) didn’t result in frostbite.
- Eat small meals or snacks. Maybe it’s the ever ravenous athlete in me, but I did NOT lose my appetite post surgery, as I expected to. But despite being hungry, I was hesitant to eat too much for fear of adding bloating to the already painful swelling.
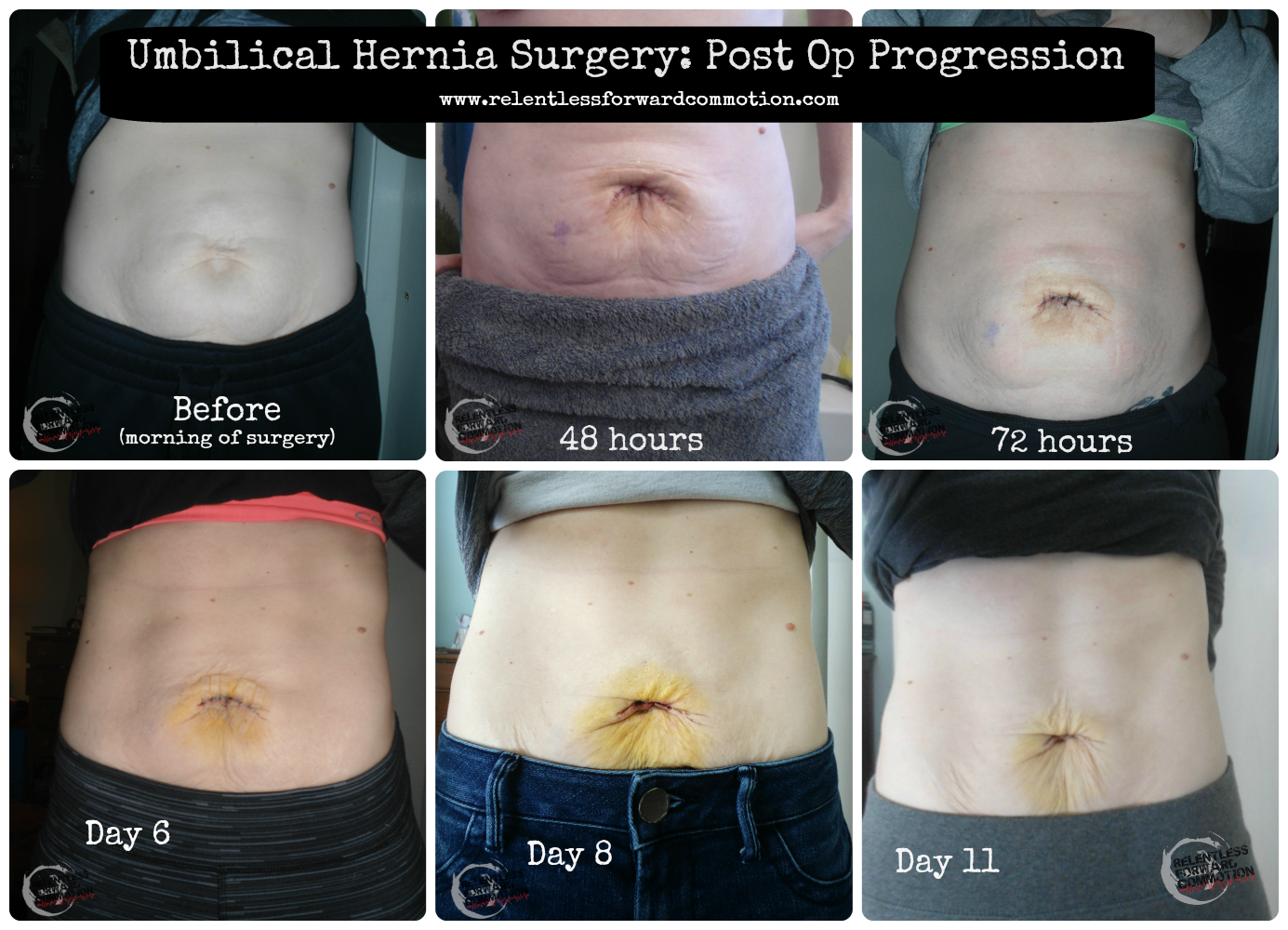
Current progression of swelling and incision. In the top left “before” picture, you can see the hernia poking through just above my belly button.
3) Bet you didn’t realize how much you use your core!
I sure didn’t, and as a personal trainer, I’m overly aware of how we use our body on a day to day basis. The tiniest thing, like turning my torso ever so slightly to the right to see what was going on beside me hurt. 11 days later and I still can’t use a vacuum to clean the floor at work. The nurse that took care of me in the hospital told me that I would become really proficient in finding ways to move about without contracting my core. She was right. So:
- Ask for help. All of the time. I constantly had Geoff help pull me into a seated position from lying down, or a standing position from seated.
- Sleep on the couch. You want to sleep on a surface that is relatively high off the ground, making it easier to get into a standing position. But the couch has the added benefit of the back, which acts as an awesome brace to pull yourself up on without overly engaging your core. I became a pro at it. Lastly, for the first two nights I didn’t even want to lay flat, so the couch arm aided as platform to layer a ton of pillows, making myself a very comfortable, nearly upright bed.
4) A pillow can be your best friend during umbilical hernia surgery recovery.
I don’t know what compelled me to do it, but as soon as I got home and laid down on the couch, I put a pillow on my abdomen. It not only felt soothing, but acted as a layer of protection between life in general (running cats, well meaning loved ones that “forget”, random flying objects) and my incredibly sensitive incision. Further, I would brace my core against the pillow when I tried to stand up and walk around for the first 48 hours. It felt really good to have that support against my sore abdomen.
5) Don’t be a hero: take your pain meds*.
I was prescribed a rotation of over the counter ibuprofen and prescription oxycodone. For numerous reasons, I don’t like taking pain pills. I don’t like the haze they put me into, nor the side affects they come with. And so, less than 24 hours post surgery, I stopped taking them. I almost immediately regretted it, and found myself in a lot of pain. My mother in law had to remind me that I JUST HAD SURGERY, and that this was what the pills were designed for. I reluctantly took the medication and slipped back into the oxycodone stupor. Though I didn’t like taking the pills, I found staying on top of the schedule for the first 72 hours made the pain far more tolerable. Further, they literally forced me to rest and relax, which is absolutely essential when recovering. Therefore, after the third day, I was able to cut back to only ibuprofen.
*as prescribed by YOUR doctor.
5) Pooping sucks.
I didn’t want to beat around the bush, so forgive the forwardness of this bullet point. But, anesthesia combined with prescribed narcotics will bind you up really fast. Add to this the that the fact that abdominal surgery makes it really hard and painful to contract your core (and thus, bear down while on the toilet). You are likely going to be come constipated, and while that is never fun, it is even more miserable post-op. Here’s what helped me:
- Hydrate, hydrate, hydrate. Drink plenty of water and other fluids. Not only does this help “get things moving”, being properly hydrated is essential in helping your body recover.
- Eat small meals, but make sure they are high in fiber.
- Ask your doctor about a stool softener. Mine recommended over the counter MiraLAX
.
- Carry a small pillow into the bathroom to brace against your core (see #4). It sounds silly, but it really helped me during my umbilical hernia surgery recovery.
6) REST, RELAX, RECOVER.
I don’t have a sit still personality. I’m not sure if this is a blessing or a curse, but “not doing anything” is NOT in my nature. Physically forcing myself to stay put, while mentally ALLOWING myself to stay put was a challenge for me. And still is, if I’m being honest. My activity limitations included, and I quote “non heavy lifting or straining until pain free”. On day #5, I felt pain free, and lifted a box that I would NEVER consider heavy (maybe 15 lbs). I wound up back on the couch that night in a lot of pain. It was too much, too soon. In hoping to be able to compete in a race I have this upcoming weekend (doctor approved) I’m continuing to take time off from exercise despite the fact that I feel great. And it has been a really hard.
But…
It is important to think of the big picture: healing and recovering now means you’ll be back to normal activity (whatever that may be for you) sooner than if you try to push too hard, too fast. Do not be afraid to ask for help from your family or friends. Let someone else deal with the house, the kids, the dogs, etc, as much as possible during the first week. As mentioned in bullet point #1, despite numerous surgical advances making this an outpatient procedure, it IS still a big deal, and your body needs time to properly recover.
So there you have it, my first hand experience with umbilical hernia surgery, and a few things I wish I had known ahead of time. As always, all concerns should be brought up with your physician. But if you have any general questions about my experience, please feel free to comment below!
** 6/8/17 Click here to read the 1.5 year recovery update***
(Spoiler alert…it came back.)
*7/2/17 Click here to read “Adventures with Ventral Hernia Surgery – Take Two” – the story of my SECOND hernia surgery.
Heather Hart is an ACSM certified Exercise Physiologist, NSCA Certified Strength and Conditioning Specialist (CSCS), UESCA certified Ultrarunning Coach, RRCA certified Running Coach, co-founder of Hart Strength and Endurance Coaching, and creator of this site, Relentless Forward Commotion. She is a mom of two teen boys, and has been running and racing distances of 5K to 100+ miles for over a decade. Heather has been writing and encouraging others to find a love for fitness and movement since 2009.

Elle
Wow! I think lots of rest and pain meds definitely are a priority here. I hope your recovery is smooth and quick as can be.
Mark Pettigrew
Were you able to climb stairs when you got home? I was told slowly
Steve
Tell me about your meds regament etc.
I was told to take Tylenol 3 …I am on night 2. Took my first stool softener tonight
Michelle
My experience:
I had umbilical hernia surgery on Tuesday May 26, 2020. I went into the emergency room and was seen at 3:00 am and the surgery was scheduled for 7:30 am. Due to my extreme pain before the surgery, I was given an injection for pain and a nasogastric tube was put in my nose and down my throat to help relieve some of the pressure. After being given anesthesia, I remember being wheeled down the hall and that was it!
I was told the actual surgery took approximately 30 minutes and after waking, I was brought to my room. I had absolutely no appetite (I had only eaten a breakfast sandwich, which I threw up, the day before). My mouth was dry, so my mom fed me some chipped ice. I was in pain, but not nearly as much as I feared. In my opinion, the pain was less than the pain after closing your finger in the car door. My pain also wasn’t constant. I got pain when I moved or coughed, which was the absolute worst! By the end of day 1(day of surgery), I was able to get up and go use the bathroom. Since I was on a liquid diet (I force drank a cup of cranberry juice and a cup of Jello), only liquid came out.
By the morning of day 2, I still had no appetite and I was really nauseated. I was given something for nausea, along with two pain pills. The pain, which wasn’t as bad as on day 1, was still present. I was able to use the bed rails to pull myself up to a sitting position and walk to the bathroom without assistance. Sitting was uncomfortable, but it wasn’t painful. Although I hadn’t had a bowel movement (the surgeon said they usually don’t release until after the first bowel movement), I was released on the afternoon of day 2. I had mild- moderate pain when I moved, but nothing horrible. I feel the post op hernia wrap helped a lot with reducing my pain.
On my first night home, I took 1 prescription pain pill and that was all I needed (the next day I took 2 Motrin). The worst part of recovery for me, was/ is (I still have a few days before officially released) the nausea/heartburn. As I stated, my surgery was on a Tuesday morning and I didn’t eat any food until I forced myself to eat on the Saturday morning. As I sit here typing, June 20, 2020, I’m having nausea and sour stomach. My stitches have been removed, my incision is healed and I’ve almost resumed normal activity, however I can’t get rid of the nausea and sour stomach no matter what I eat. I should note that I dad my first bowel movement on the Sunday after surgery. Unlike many that I’ve read about being constipated, I had diarrhea for the first two movements.
Overall, although I wasn’t planning on having the surgery when I did, I’m happy to get it over with and I’m going to do what I can to make sure I don’t get another! It wasn’t as painful or scary as expected (this was my first surgery) and I’m happy to be able to walk around, without fear of my hernia popping out and causing pain.
Jim
I just had umbilical hernia surgery this morning. I wish I had read this article before then. I am in lying in bed and hurting. My biggest question right now is what is the best way to get up from laying down. Since Doctor said To not do sit ups, I am trying to roll on my side and roll off the bed. Thanks for your insights. Very helpful
Ryan
I’m on day 8 of recovery and I’m so glad I found this… I’ve experienced all of this too and not sure if it was normal as I don’t know anyone who has went through it.. I’m 29 and my god it sucks being stuck in practically incapacitated. The weird thing for me is the sensation.. not sure if you feel the same but can you feel the mesh inside you? My belly button feels hard under the dressing and when I move it feels like something is moving under my skin. A feeling I’m hoping will go away over time! I live in a top floor apartment with NO LIFT also so, I’ve pretty much been locked up here alone like repunzel for the past week. Really glad to find this though I just hope mine doesnt come back like yours because FUCK going through this again. I can’t wait to get back to to normal so I can at least do cardio at the gym… I feel out of breath just getting up off the bed now! Wtf is that about?!
Mike
Wow this is unbelievably well-written, thorough, and descriptive, in plain “normal people talk.” Lol I just had mine 4 days ago snd this is really accurate. Thanks! Nice job.
Sree
It really helped me. Thanks a lot
Aminat B
Hi
What abiyt the mesh……. did that hurt? Did you even know ut was there? How did you get your diastasis down to 2 fingers…… mine is a 4 finger
Judy
I really enjoyed reading your experiences. I had an incarcerated ventral hernia repaired 2 weeks ago. It went well and the real pain has subsided and I was feeling almost normal until 2 days ago when I started having some of the symptoms of the hernia again–heartburn, nausea, bloat and feelings of fullness. I’m hoping I’m again having these symptoms because I’m still swollen post-surgery, but it’s weird that I haven’t had these issues until almost 2 weeks into recovery. IIts concerning me enough that I’ll probably contact the Dr. tomorrow if these symptoms continue.
Melissa
I felt the same way!! Recovery was way worse then expected. I was told paid for only 48 hrs day 3 here I am still in pain. I couldn’t walk up stairs the first two days, I could barely breath and I was having a hard time talking ! I recommend stool softeners or laxative because there’s no way you’re going to the bathroom!! Bring a pillow forsure and try not to push! This was not what I expected and hopefully it gets better soon! Thanks for the read it was nice to be able to relate!
Lylah
Thanks for all the advice. I just got mine done this morning.. it sucks and had issues getting my pain meds right after surgery. Luckily i have help but as a mother of 3 it’s hard to ask for help or let anyone do anything for me. Thanks again. I’ll def be taking a bunch of your advice.
Manga Lady
Hi thanks for the post. The worst part of it for me is the severe muscle spasms. They are the worst i have ever experienced. Pulling on the stitches and tearing the flesh, well it feels like it. Searing pain ripples along the umilicus all the way around to the external obliques. In my experience opiates DO NOT help with this pain YOU MUST USE A MUSCLE RELAXER. I use 5 to 10 mg of BACLOFEN, which must BE TAKEN WITH FOOD. If BACLOFEN is taken on an empty stomach it does not work.
So muscle relaxers will help you much more than opiates.
And take that 4 weeks NO HEAVY LIFTING seriously, also NO PUKING. Puking tore my stitches also.
Great article,
R.
Rosie
Man I’m so glad you posted this .. you are not kidding about the swelling.. I am currently day 7 post op. I had asked my doctor about using a waist trainer, which they did not recommend. So this is the first time in months I have seen so much bloating. Yes I know some people are against waist trainer but they help me keep water weight away. So I put my waist trainer I forgot I had it on so I take it off after several hours and why do I see my stomach yellow, I’m freaking out and I see your recovery pictures and mine looks exactly alike. You just saved me from a meltdown
David Robinson
It’s been over six weeks since my surgery and I still have pain. Oh, it’s not as bad as right after surgery but it’s a pain that’s with me the majority of the day. My doctor told me that orthascopic surgery,although less invasive, causes. Much more trauma than the open incision procedure. Like you,the doctor who performed the procedure said I would only have pain for a few days. Now I’m reading nightmare stories about people who have had pain for over a year and a half.
Heather Hart, ACSM EP-C
Hey David! While everyone is different, I definitely experienced some discomfort and occasional pain from the stitches/scaring healing for a few months. I am now 4 years post op from my 2nd hernia surgery and have zero long term lasting issues. I’m as active – if not more – than I was pre-surgery. (And I agree that the recovery from laparoscopic surgery, which I had on my second repair, was FAR more painful than the open incision I had the first time!)
Maureen
I hope you continue to recover at a quick pace! I’m glad you were able to ask for help…it’s hard to let things go, but sometimes you just have to take care of yourself!
Brandy
Thank you for taking the time to share this. I found this to be very insightful. I am on week three of a double umbilical hernia repair & it has been hella-painful….
Ivy Shelnutt
Hi I had the umbilical hernia surgery about a week and a half ago. I was wondering is it normal to get a sinus infection after the surgery? I seem to have gotten one and it started with a headache behind my eye and now it has moved to my cheek. Is this normal? What should I do?
Thanks,
runprincess80
I am sorry to hear about this. I hope that your recovery continues to go well. Take it easy and give your body time to recover
Ange @ Cowgirl Runs (@cowgirlruns)
Glad to hear you’re almost back to 100%! I’ve only ever had surgery from broken bones, but knowing how rough those were to recovery from, I imagine any abdominal surgery would be difficult. Hope you continue to get back to your regular self 🙂
Nicole @ Fitful Focus
I’m sorry it’s taking you longer than expected to get back to 100%, but I’m glad you’re not trying to push yourself too fast too soon.
margodono
Hey there! I disagree in only that I love pooping! Not being able to poop is the worst!!! Feel better. 🙂
Kate @KateMovingForward
This looks like a tough road, but great for anyone looking to know what to expect. Hope you are feeling better soon. 🙂
NutriFitMama
Oh man, surgery and recovery is ROUGH!
Sue @ This Mama Runs For Cupcakes
Great post. A lot of these tips go for people who have had c-sections as well. I remember I had a pillow by my side for a while after my c-section. The belly looks great though!
Patty @ Reach Your Peak
I’ve never had surgery (knock on wood) but can imagine it’d be scary and recovery would be a pain (no pun intended haha). I hope you are back to 100% asap! As someone who’s really active I’m sure it can be frustrating, especially lifting something you didn’t think would be heavy at all. Good luck in the race this weekend!!
Marcia
Sounds like this has been a long, rough road. I’m glad the worst is behind you and wish you continued healing and recovery.
Kathryn @ Dancing to Running
I hope that your recovery continues to go smoothly and as quickly as possible. Its never any fun to be stuck at home and in bed, but you seem to be managing the recovery as well as you possibly can.
Raghvendra
How many weak take the rest after umblical harnia opration.
jillconyers
Dont fear the pain meds! Well said. I’m not a big proponent of medication but there is a time and place that it is necessary. Why suffer if you don’t have to.
A speedier recovery to you!
Ivy Shelnutt
Hi I had the umbilical hernia surgery about a week and a half ago. I was wondering is it normal to get a sinus infection after the surgery? I seem to have gotten one and it started with a headache behind my eye and now it has moved to my cheek. Is this normal? What should I do?
Thanks,
fitmomintraining
LOL, Pooping sucks! That’s how I felt post c-section. And after my second, I had a horrible sinus infection, ear infection (bilateral) and would have given anything to not cough, blow my nose or sneeze.
Heather
Aww that’s miserable! Yes, I sneezed once out of the blue, and was overwhelmed with how painful it was!!!
runningbuns
This is so great. Thanks for hashing it out. I’ll be coming back here when I take the hernia surgery plunge!
Kasskdy
I’m day six and idk if I’m swelled or I the hernia is back!
amanda polchies
I don’t know if you check this periodically or not but this was a big help I’ve had my hernia for 4.5 years now ever since I had my twin daughters. My doctor told me I had nothing to worry about, that it wasn’t the type of hernia that would grow in size LIAR it feels huge and at times I swear I can feel the thing pulsating and it does it so hard at times that it brings me to tears its horrible. I will be calling the doctor tomorrow to officially set up my appointment for surgery I hope they can schedule me for spring break that way I don’t miss much of my college courses. Thank you so much for posting this it has been very informative so far the best once I’ve read it def helps but its scary I had a csection and didn’t have to take my oxycodone I just took ibuprofen and the same with my wisdom teeth I hate the things so I will probably suck it up again and just take the ibuprofen lol one again thank you so much for posting this it really helped,
Sp
Thank you for this! I have my pre-op in a few days for the same procedure and I was completely psyching myself out reading about mesh and hernias online. I was hoping to find a positive review from a fit mom in my age range for some reassurance that things will probably be fine! Thanks again 🙂
Heather
You are welcome! Best of luck with your surgery! All things considered, it wasn’t nearly as bad as I expected. I’m already back to doing what I did pre-hernia. Hang in there!
Amy
I stumbled over this post as I am on day 2 after my hernia repair. I didn’t get the mesh. I too am a runner and am anxious to get back out there. Thanks for your honesty about taking it easy, I needed to hear that.
Valentina Turcan
How was your recovery? I’m looking for reassurance or not before taking the plunge but with a no mesh repair.
Jennifer
thanks for sharing your experience! I am on day 4 post op. I had laparoscopy with mesh. I really fooled myself about recovery- assumed I would be fine by day 3 or 4. Not the case at all. I too have a really hard time sitting still. But I am sitting a lot because getting up is not fun. Once I’m up it feels less painful but I’m so tired and weak.
Your story has helped me realize that we all heal at different rates and I need to be patient and think positive
Glen
So glad I stumbled upon this. I recently had an umbilical hernia op
And have a hard lump bigger than before. I was becoming really worried until I read all of the above comments. We all appear to have had the post op problems that are largely nothing to be concerned with. I shall sleep better tonight. Thank you all for your help.
Jena
I had an umbilical hernia repair open surgery 5 days ago. I was shocked when I awoke in recovery as I was informed of small lasik incision. However, the incision is from breastbone to under my navel. Extremely bad cut. I can honestly say the last 2 days have been MUCH EASIER. The first day hurt tremendously, second was worst. Sneezing, coughing, throwing up, all is HORRIBLE PAIN. Using the pillow against the wound DEF HELPS. It’s a MUST DO. However, getting in any comfortable position to sleep is impossible, still 6 days later. The worst for me is how swollen my stomach is. I anyways been a small framed person. I can pass for 7 mths pregnant. It seems as though I can feel something moving around in my tummy area. Eating makes bloating HORRIBLE on top of swelling. My ribs literally hurt the most. Feels like there stabbing something inside me. Like there’s no room for everything Bc of swelling. My belly gets SOOO HARD and that’s quite painful as well. Laying flat on back feels like your tummy will blow out. My ribs and muscles are aching HORRIBLY throughout the day BUT at night while TRYING to sleep on either of my sides in attempts to be a little comfortable to sleep. This occasionally works and sometimes it makes me forget the pain. Then other times it makes the pain in my ribs SOOO BAD. Again like somethings gonna make em crack open…. I get stitches out tomorrow and that I am the MOST SCARED. I don’t know how I could stand this pain.
Melvina
Thank you som very much for the post with tips. I am scheduled to have an umbillical mesh lap surgery in 4 days. Ive been trying to prepare myself mentally. Ive been trying to figure out the best place to sleep in a bed or on my chaise lounge chair. It sounds like the lounge chair will be better so i dont have to come from a completely flat position. And the pillow on the tummy, very helpful tip.
Melvina
Had my hernia mesh laposcopeic surgery on June 24th 2015. I wore a zip up terri cloth type cover up (the length was simlilar to a short dress). I wore flip flops and no under garments because they make you take them off during the operation and i didnt want to bother trying to put them back on afterwards. The Terri cloth material was perfect because it was like being in a robe. Everything is covered and no one could tell i didnt have on under garments.
After surgery, all i had to do was zip up and slide on my flip flops.
Pain….OMG!!!! I dont know how to describe the pain but let me just say the pain medications 5mg of percoset and 350mg SOMA were like baby asprin. I had to take two percosets at a time just to get a little relief. My doc prescribed 50 percosets with directions 1-2 every 4-6 hours for pain. I had to do just that 2 pills every 4 hours even during the middle of the night.
I was out of pain meds in 6 days needed a refill.
FYI-I will admit i HATE PAIN my tolerance for it is not good. Could be a factor too. Howwver, I dont drink, smoke or do any type of drugs ever so you would think the 5 mg would work….but it didnt.
Anyway just know its painful especially getting up, walking, even taking deep breaths.
Standing straight up was impossible for me for the first 3-4 days.
I’m about 12 days in and im still struggling with standing up straight and walking for a long period of time.
About a week before my surgery i started experimenting with pillows and places to sleep that would make for easier transitions when standing. The chaise lounge chair offered the best options over my bed or couch. I set up everything two days before surgery.
I slept on my chaise lounge chair and put my futon matress under the lounge chair pillow to make it a bit higher (then put a fitted sheet over it) which helped when sitting and standing. with a few pillows to aide with different positions.
I slept with a short tank style shirt and no underwear so i wouldnt have to bend over to pull them up and down. Because I had to drink alot of liquid i had to pee alot. The distance and pain just to go to the bathroom (especially through the night) was so bad my husband cleaned out a plastic 16oz juice bottle and i started using it too pee in. I would just slide down the side of the lounge chair and hold the bottle while squatted. This made it so much easier (my husband still had to assist with me getting up, emptying the the bottle, etc.
I used fiber in my food, took milk magnesia and stool softners to make sure the pain meds would not constipate me because just the gas forming in the stomach hurt. I ate oatmeal, raisins, bean and chicken noodle soup, small sandwich, ice cream, lots and lots of gatorade and water the first couple of days. My bowel movements were always easy no straining or constipation.
I keep the ice pack on and use ibrupropen in conjunction with my pain meds to help with inflammation.
i apply the pain cream and inflammation pain cream 4 times a day.
Im only having to take pain meds like 2-3 times in 24 hours (if ive been moving around alot it seems to cause spasms).
I hope something in thia post is helpful.
Melvina
This is Melvina again i just wanted to add that i am 47 years old in good physical and mental health with no other illnesses. Im 5’6 146 pounds so my weight is fine for my size. Im not an excercise guru but im not a couch slug either. However, I think it is important for me to mention my age and my absence of consistent exercise which may also be a factor with me not being further along in the recovery by this 12 days.
Dick
Thanks for your post–I’m ten days post surgery and I feel like my pain is getting worse. I have really taken a step backwards and my pain is tough to get under control. I am trying to make it through without the prescription pain meds–bad experience from ACL surgery–so am using Tylenol and Advil. I feel like my ability to bend, etc. is getting worse. In addition, I now have a hard doughnut-like swelling around my navel that seems to be growing a bit. No redness on the outside to show infection. I just scheduled a doctor follow-up for Monday (It’s Friday) as this just doesn’t seem to be normal.
Heather
Hang in there ! It does get better after about a month. Glad to hear you made a doctors appointment, possible infections are nothing to mess with. Good luck to you!
Jennifer
Hang in there! I remember having similar pain and wondering why it’s not letting up. It took my abdomen about 3 weeks to feel like I wasn’t pulling every muscle when I would get up from sitting or lying down. I am now 8 weeks post op and I finally can say I forget about it most of the time. Good luck yo you
Melvina
I hope everything is ok. Did you have lapascopic or open sugery?
Michelle
I really hope everything was sorted for you and you made a full recovery.
Michelle
Your post has been very helpful. I had the exact same surgery procedure and i am also on day 12 of my surgery, and still feeling pain. I take panadol pain killers at least once a day if it gets too painful for me. Luckily i can stand up straight but i feel very tender still, and when i walk, my entire abdominals feel as though they have bloatedness, and it gives a heaviness sensation, especially when first standing up. I thought that by now, nearly 2 weeks later, all these sensations would be gone by now. But i also had or still do have, an infection that could delay recovery. Have to take each day as it comes i guess. I have to keep reminding myself that its only been 12 days, and this was a major operation for me, due to the size of my hernia and my obesity.
Brenda
I am 62 and single. I was just told I have a hernia. I’m calling my doctor tomorrow to set up an appointment. I have had several surgeries over my live time but it sounds like this could be the worse. I can’t handle pain at all. I will not have any help. Well maybe a little but most of the time I will be completely alone. It is nice to read all the postings so I know what I will be going through.
Richelle
Thank you so much! I just had surgery and i am doing all the same things. I appreciate you cutting to the chase. I am 1 day post-op and was thinking of lessening my needs. I will wait. Sleeping all the time and propped up on the couch like you wrote. Passion meds giving me headaches and make me so sleepy but i will deal. Good luck to you.
Daniel Francis Gardecki
Tip 7) You will probably get a swollen foot. Had my hernia repair 9.5 days ago.
Took my cocodomol regularly for the 1st 4 days, then once or twice a day after.
Wore my stockings for 4 days to be safe (instead of the 2 they recommended) to prevent a blood clot. Went for a check up on day 5 because there’s still a lump in the middle (my hernia took up most of the right of my bellybutton originally), but apparently its normal and will ‘probably’ shrink.
Then halfway through day 6 just as my mobility is getting back to normal, I get a massive shooting pain in my foot, and now on day 9.5 its swollen and still painful.
I’ve done a bit of Googling and it could be an edema, but if it is, it should be painless, which mine isn’t.
Painful foot pain usually has something to do with diabetes, pregnancy (I’m a 29yo man), kidney disease, liver disease, anaemia, increased salt intake, phlebitis or venous disorders of the legs like Deep vein thrombosis/drug allergy.
I’ve always had random pains in my legs/feet usually in my joints, but everytime I bring it up the doctors always rule out things like arthritis and say “Its normal”, and after all my recent blood pressure tests, blood tests, urine samples, and ECG’s, they’re all perfectly normal too so I’m confused.
I’m sure its related to the operation as other people who have had umbilical repair operations have had the same painful swollen feet/foot but I can’t understand what the cause is.
Looks like I’m off to the doctors in the morning.
Katie
Thanks for this! I had surgery for inguinal hernias on both sides on Monday and am finding the recovery to be a lot more intense than I had expected. Also, I’m super active too, so it’s hard for me to not do anything. I’m going to be rereading #6 multiple times a day. I need the reminder.
Piilani
Very good information! I have recently had umbilical hernia surgery, on day 5 now. I finally stopped all medications, and am walking better. I used pressure applied with my hands to provide counter action when trying to move. I concur on all points regarding use of the core and needed to be reminded to avoid carrying things. I used a laxative + stool softener which was very necessary as you do not want to push to avoid hemoroids and any abdominal strain whatsoever. The bloating is very obviouse although I thought I was fat from the inactivity. So it was good to hear that bloating is usual. I also noticed that I didn’t feel comfortable laying flat at first and felt the need to brace my abdominal after eating. Thank you for sharing your story!!
Char
After trawling through breezy recoveries and horror stories this article helped me feel better. Day 3 in a lot of discomfort, look pregnant but still hungry… Was not a personal trainer before but hoping will see brighter days next week. Well explained….now if only I could go to the bathroom…..
lynn grieff
I han umbilical surgery 6 days ago and we
hen I eat (little) my belly hurts. Is that normal?
Adri
Your blog is what I’m going through right now! Hope you are doing well,
susan Auvinen
I had my surgery three weeks ago. I am very unhappy because I’m unable to Jazzercise and I see my fat coming back. Previously I would do it six times a week over the last three years and lost a lot of weight. I can’t zipper my pants and they have to wear sweatpants to my accounting job and it’s very embarrassing. Suddenly my stomach feels really big and the new skin and the new bellybutton is very sensitive. I still can’t fall asleep without 100 pillows on my bed I live alone and don’t have anyone that could help me. I don’t know how I’m going to go through another three or four weeks like this. It doesn’t hurt it’s just that I’m tired of using my arms and my legs to get off of couches and off the bed and into the car.
Bill
Well, not what I expected, but needed to hear! I am 63 beer bellied male who experienced this dilemma as a result of hard work around the house, such as building a 800sqft patio. Had 4 pervious knee surgeries, including one 30 yrs ago which was a ayear recovery and very painfull. Thought this would be easier…but now!!! Getting cut on Thurs 8/13/2015. Your posting is the only one I found; so, THANKS. My wife returns to the classroom on the 17th, so I have a nurse for 72hrs. Pillow sounds like a great idea. Know what core is needed for everything, as I was a gymnast in BK TIME (Before Kids). Thanks again. “I’LL BE BACK!”
Heather
Good luck with your surgery Bill! Hang in there, the first day or two are tough but it gets better fast! Thanks for stopping by!
Jennifer
Good luck Bill. As others have said it may be rough at first but each day is better( even if it’s only a bit better)..be patient and think positive.
Bill
Update: Surgery was 8/13 with cutting on the dotted line at 1:30ish in the afternoon. On the way home by 4:30. Sore and concerned about movement, ride went well. First evening my wife had to help me up and down as I lived in her recliner. I think the key for me was ICE PACKS!!! By 2AM I could get out of the recliner without help. I kept ice on 24/7 for the first 24hrs, and then as often and as long as possible thereafter for three days. Friday at 4PM,we went to a memorial for a great friend and I was on my feet for 3hrs. Still not too bad. Hosted an impromptu family gathering with our three children and 4 grandchildren with a total of 12 in all. Made 6# of venison barbeque in the afternoon. I am telling you all this to confirm it went rather well. Biggest problem I had was CONSTIPATION!!! Finally resolved this Sunday 5AM, after multiple doses of softeners and finally Ducalax! Drank plenty of fluids. Took pain pills for the first 36hrs and then nothing. Today is day 4 and I am handling max of 15#. Still taking it VERY EASY. Did some wash today. Bending over is the toughest thing at this time..
My suggestions are: Stay off your feet as much as possible for first 24hrs. ICE, ICE and more ICE. Take your pain meds to stay in front of the pain until you are in your comfort zone. Keep ICING!!!! Stay under the lifting limits and do not stretch overhead or bend excessively. Do get up and walk around, including stairs as this will help any air in side your wound to be moved around and absorbed.
Good Luck and keep moving.
Melvina
Just wondering if you had open surgery or mesh? With your very quick ability to move sounds like an open surgery because the mesh had me out for about 9-11 days easy.
Heather
Melivina, personally I had mesh! Not sure about Bill!
Heather
Bill, so great to hear your surgery went well! Yes, constipation was one of the worst parts, no doubt. Thank you for sharing your experience!
Georgette simon
Did you have massive indigestion?
Georgette simon
Have not been sick to stomach, just nasty feeling indigestion
Melvina
It’s Melvina again. I had my umbillical hernia mesh surgery on June 24th 2015. Im experincing sharp pain like glass or knives cutting inside. The pain comes and goes but OMG it hurts like nobodies business. Is anyone else experiencing this or has experienced this?
Michelle
Yes, i had sharp like stabbing pains while i was in hospital and several days later, they said i had puss due to infection. Yesterday and today, i’ve experienced some sharp pains around my hips, and in my back for some strange reason. Its like someone is knifing me in those areas, though how could that be because my surgery was around the abdominals, not my hips and my back. Its weird.
Melvina
Im still getting the sharp glass pain. my surgeon who has responded colder than dry ice by simply stating it has nothing to do with the surgery. He never took the time to touch the area where the pain is occurring on my lower abdomen. He only states no one has ever had a problem in the 10 years he’s been performing hernia surgeries. He wasnt even willing to believe it could be my body having a difficult time healing or scar tissue. Im so frustrated. Not sure if it could be the sutures inside pulling or what is causing the pain that usually occurs when i stretch. The area is sore for days after that. Help anyone.
Lee Strausberg
Get a second opinion from someone not in the same health system.
Melanie
Hi
I’m nine days after umbilical and femoral hernia repair
Still lots of wind pains and discomfort when walking
It’s good to know I’m not alone
Feel well soon
Harriet Weinstein
Thank-you for your great post. I really appreciated your candid and informative comments. I am a 63 year old woman who just had open umbilical hernia repair (with mesh) 7 days ago. I usually handle surgery pretty well. I have had multiple surgeries over the years: 3 hernia repairs, adhesion surgery, uterine cancer, 2 ovarian surgeries, tummy tuck, meniscus repair, carpal tunnel etc. I had a major rectal prolapse surgery in May. I still haven’t recovered from that. That was hell. I will have a ruptured tendon in my elbow repaired in November. I guess I should donate my body to science when all this is said and done.
Recovery with this hernia surgery has been more or less uneventful. My surgeon told me to take walks, not lift anything heavy, don’t reach up with my arms to take something out of the cupboard, etc. I forgot to ask him about going on a recumbent exercise bike at this time. What do you suggest? Is the problem with overdoing it due to the actual physical movement, the raising of the pulse, and/or increase in blood pressure?
Best wishes
Lindsay
Thank you so much for writing this. I had open surgery with mesh 5 days ago, and my stomach is very very swollen and I was beginning to get worried about it not going down (I am getting married in 5 weeks and need to get into my dress!!). So pictures and descriptions from everyone has been really helpful and quite reassuring too.
With regards to pain relief, I have stuck to paracetamol and ibuprofen for pain relief but recommend to other to manage the timings of it better (than I did initially) for controlling the pain rather than have to react to it. The pain for me is ‘inside’ rather than the scar itself (which is absolutely fine and seems to be healing nicely.)
Thank you to everyone for their comments on here too – they are all good to read.
Roy Russell
did you ever have a hard mass in your umbilical. Its not like solid but far from liquid
David
Hi Roy, yes its normal. The firmness an swelling are part of the healing process. I am three weeks post op and still have a small ring of firmness around my navel.
My hernia was done at the same time as an emergency appendectomy. So I’ taking it real slow.
Jessica
Thank you for sharing. I hady surgery today, with mesh, and wanted to know of this much pain was normal. I work out too and lift heavy weights so I will heed your advice and allow myself to heal. And I will be trying your pillow tip!
Thanks!
Sem
Thank you for this: I’ve undergone the same procedure 24hrs ago and everything you’ve written so far sounds very familiar to me i.e the expected recovery time from doctors, and it really did come as a surprise to me at how much we use our core!
Thank you for your honest blog as it provides a realistic perspective.
Trisha
I found your posting really helpfull, so informing very too. My husband has same kind you had. Now my husband is talking with his Dr to get his fixed. Worried about how long he will be off work is concern for him. You take care and God Bless.
Sarah
Hey everyone!
I will be four weeks post-op tomorrow and have noticed a marked increase in pain along with some swelling right below my belly button. The area is also very tender, with some spots of sharp pain when I press lightly on it. This was not the case a few days ago when things felt pretty good. I had the procedure done open, no mesh (doc said it was too small for mesh), and under local anesthesia (don’t remember a thing, thank goodness). Things seemed to be progressing and I had a post-op appointment last week. Everything looked good then, but they started going downhill three days ago. I called my doctor and they seem to think it may just be normal inflammation from increased activity. The surgeon cleared me for light activity after my post-op appointment and I have been doing some incline walking on the treadmill and light (<8 lbs) weights for bicep curls and triceps extensions (all arm work). Nothing I've done has spiked pain. Rather, this has been a somewhat gradual increase not tied to anything in particular. Has anyone else had this issue??? I'm trying to trust the doctor, but am extremely uncomfortable and am worried that things are not healing properly or I may have damaged the repair!
Hadeel
Hi. I noticed that you wrote local anesthesia, please explain.
Helen
Thank you!!! I’ve just had a hernia removed, four days ago, although it feels like forever ago. Pushed things too hard yesterday trying to look after my toddler, and have ended up back in bed today, feeling pathetic. It’s good to know that it’s normal, and I am indeed allowed to rest. Truly is resting is so very difficult to do. Great blog, really helpful xx
Danielle
Had umbilical surgery september 11th 2015 no more pain today accept a small lump above my naval it hurts is this normal
Michelle
Today is day 12 of having Laparoscopic Umbilical Hernia repair and spent 3 nights in hospital. The first night was spent in ICU. I am also obese, and find that i am still feeling very tender and sore on and off. I also have an infection that i am being treated for with prescribed antibiotics. I really hope they will rectify this infection. I really do not want any more complications or having to need another surgery or to lose the mesh. My hernia was very large and i need that mesh for the added strength. Post surgery, i was draining for nearly a week and needed my dressing changed every 2-3 hours. An infection was found present, hence why i am being treated for it, and another incision is also showing signs of an infection. I go back to doctor this afternoon to assess my wounds. I don’t have a fever and i have an appetite so its probably not too bad, though i can’t help but think “Will i succumb to this infection or will i fully recover?” I am trying to remain positive. Though the tenderness and slight burning around the navel adds to my worry. Anyway, i thought i would share my experiences with an umbilical hernia repair. I find that i can walk but can’t do a whole lot yet. I have to keep reminding myself that its been less than 2 weeks, and due to my size, i have to expect recovery will take longer because this was major surgery for me, due to my size and my hernia size.
Loved the article.
Jennifer Piggott
Hi thanks for your post. I have a small umbilical hernia but my diastis recti is bad too can you tell me have you got a flatter stomach now after repair?
Heather
Hi Jennifer! I found I had a *slightly* flatter stomach simply because I wasn’t constantly feeling bloated from the hernia. However, my DR was/is only about 1-1.5 fingers. If you have a severe DR, the hernia repair will not fix that 🙁 Have you talked to your doc about having the DR repaired as well?
Gina Hayes
I’m going in for a surgery consult today and am very hesitant. Your before picture looks exactly how I do! Anyways I’m a gym rat like you are. I lift heavy 4x a week and also run. How long was it before you were able to lift weights again and resume your normal life ?? I really don’t want to be out for 6 weeks!! I don’t know what I’d do with myself if this is the case and may not go ahead with the survey. Also is your stomach flatter and better now that you’ve had some time after the surgery to heal!! Are you happy with the results?!
jamierantz
Thank you times a million for wiring this. My situation is very similar to yours…I am getting my hernia repaired in December. I am 29 and have two children, I run 25+ miles a week and have been focusing on core strength knowing that I will soon be out of commission for 6 weeks. I have never had surgery before, so that scares me crap out of me. Are you happy you did the surgery?
Mark
Thank you for this. I too do not have a ‘sit still’ bone in my body. My job is active (glass blower, a very physical artform). My hobies are active as well, running, rock climbing, cycling. I’m struggling to not over exert myself and prolong my recovery – inguinal and umbilical hernia surgery. Day 7 and counting….
Boone
thanks for posting this! i just had a hernia repair and had NO Idea I would be this incapacitated!
Cassandra Hill
Thank you sooo much for posting this. I am 29 years old and have 4 children so I was wondering what it was going to be like after the surgery. Mine is scheduled for November 12th and will be getting the mesh. I really love how detailed you are about everything. I am a person who values honesty about situations. I am not a person who likes to sit down for long periods of time so I will have to imagine this is going to be very hard on me. When I gave birth to my youngest who is 13 months old now, I barely sat down in the hospital or when we returned home. So this will be crazy for me. Reading your story and the responses is putting my mind at ease so that I know what I can expect.
Daniel Soto
Thank you for taken the time to write this article on your experience. Your time is deeply appreciate.
Richard
I’m a 46 yr old man 6ft 5 and 16 stone pretty active now on 4th day recovery from a double umbilical hernia op of which was open stitch up no mesh no keyhole ! Small pain but only by belly button ! Have itching and a little bruising and I took my meds 3 times a day ! Have been walking and bending but first 2 days was bad and couldn’t sleep on either side ! Some bleeding as well . My advice don’t stay put too long move about and rest again it will speed up the recovery eat a balanced diet and drink water milk and oj ! You know your body so if something feels wrong slow down !dont be afraid to ask for help and don’t lift . X
Raymond
Thank you very much for this post! I’m not a runner or avid athlete but knowing your recovery times were more than I was expecting is incredibly helpful.
Ms
Very helpful, thanks.
Sam
You look great..I look like your before and every surgeon tells me I’ll need a full tummy tuck but yours looks fantastic
Amanda
Thank you so much for posting about your experience. I am not a runner but was looking for other people’s experiences and there aren’t many out there! I just had my surgery three days ago. I had laprascopic umbilical hernia surgery with mesh. The one thing I wanted to add for others having the surgery done laparoscopically was about the intense gas pains. The first night I woke up around 4am with unbearable pain in my shoulder blades. I called for my husband to help move me and he thought maybe it was from how I was propped up on the couch. I went to dr. Google and found out that it is normal after having a laprascopic surgery. Wish they had warned me about it before hand. The gas pains were worse than the actually surgery pains. Took about two days for it to finally start to go away. Also, I was vomiting and dry heaving a ton the first afternoon. Called my surgeon and the Dr on call called back and said it was normal and to try to wait it out till the next day. But I insisted that I needed something since I couldn’t keep the pain medication down and was really in agony. Got Zofran and that helped tremendously. I would recommend at least getting a prescription for it in case you need it after surgery. I think it would be beneficial if they kept you in the hospital for the first day or two. But I guess the insurance companies don’t want to pay for it. So make sure you have 24 hour help for the first couple of days at least.
Michelle
Thank you so much for this. I have been looking for any information I can get on this surgery since I think I will have to undergo it soon. I have an umbilical hernia-getting the ultrasound to confirm it today- and I am really uncomfortable. I am so tired of feeling bloated and of having to be so careful bending, lifting, etc. I have a hard time buttoning my pants, because it makes that area of my stomach sore. I am SO ready to just have the surgery so that I can have my life back, but yet I didn’t realize there was so much involved in the healing process. I figured I would feel much better in a day! Goes to show how naive I am. I am already thinking about how I will get things done if I am laid up like that! I, too, am a busy body and hate sitting still!
Michelle
Also, this may be a dumb question, but how long before you can bend straight down with knees? I am wondering when I will be able to do things in moderation…..I want to get the surgery done ASAP, but I honestly didn’t realize I would be laid up like this.
Michelle
How did your surgery go? I had those same symptoms in November and wasn’t diagnosed until now. I had a bunch of tests for other conditions. The docs told me it was a cyst I had and that I had two different things going on-as far as the pain, it was ruled as abdomen strain. All this time and I see the surgeon for a consult and he says it’s either a cyst or an incarcerated hernia. So this has gone on for a while. I scheduled surgery, but I’m scared because of not knowing how my body will react. I hope I’m one who will feel better in a few days, but that probably won’t be the case! How did you do?
Melissa
Oh my days, finally found a blog that actually describes the way I’m feeling right now so thanks for such a detailed blog it’s nice to know I’m not just being a whimp im 28 yrs old with one child aged 7, i had my ubilical hernia repair yesterday afternoon but all did not go to plan as it turned out it was terribly infected and was a lot bigger then expected, but because I had a bad infection they had to dig it all out which then led me to being unable to have the mesh as this would have caused other complications.. So the chance of me having a recurring hernia is likely. I woke up in absolute agony I definitely think this operation is a lot worse then what they make out it to be, but I’ve kept taking the pain killers and antibiotics prescribed and I’m hoping to start to feel better in a few days, absolutely dreading taking off the bandages as I’m no good with blood, stitches ect. Hope everyone has a speedy recovery x
Steve
Hi, I’m at day 3. Thanks for the pillow tip, it works like a teat. 🙂
Jack Kelly
Had a very different experience I am currently 2 days post op had repair with mesh. First day and a half I was in a little pain. But the shots they gave me lasted prob 12 hours. Day 2 I woke up with almost no pain I haven taken pain meds for today an won’t be needing them for sleep. I’m scared and anxious for medical stuff but this was a breeze. My only other surgery was 4 impacted wisdom teeth, which kept me in pain for two weeks. I’m sure it’s different with everyone, so I just wanted to add my story o a pretty easy univentful surgery. Anyone considering surgery I would suggest the sooner the better.
cal
Thanks for this….I feel a lot more relievrd after seeing your pictures that my horrible swollen mess of a stomach (day 2 after surgery) may end up looking normal again! Good luck with complete recovery xx
Katrina
I am on Day 3 post-op and just can’t get comfortable…the “pillow trick” does help though. I had the lapy with mesh and they sewed the hole, caused by the hernia, closed. Apparently, also a lot of scar tissue built up around the belly button/hernia (presumably from c-section child birth, although my “baby” is 17). Doc said he removed a lot of stuff that shouldn’t have been there. I stayed the night in the hospital on heavy pain meds (including Morphine). I’m home now, but just don’t want to move, other than having to go to the bathroom (still have yet to poop). Although, the nurses all told me that I should walk around and it would help. I’m currently in pain and miserable and only taking Motrin 800, due to the loopiness/nausea/hot-spells/itching effect that the Narco had on me. I’m not sure which is worse. I’m 49 and normally fairly active, but no running or anything. Just thought I’d weigh in on my experience, since this has been a helpful post for me. thx!
freemyheart
I had the same issue because the doctor mistakenly only prescribed Percoset which only makes me nauseous (doesn’t seem to do anything for the pain.)
After a phone call, I was switched to Vicodin and prescription strength Ibuprofin. I recommend to anyone else going through this to let your doctor know if what they prescribed you isn’t helping. I cringe at the thought of only taking over the counter painkillers after this surgery. I am hoping that you’re feeling better/back to normal by now.
With that said, keep this in mind for the future. I knew this from a couple of years ago when I had a root canal procedure. Unfortunately this time around when they prescribed Percoset, my friend was picking up my meds and I didn’t know that they had prescribed the wrong painkillers for me. Best to get that sorted out *before* you leave the hospital. (Speaking to those that haven’t had the surgery yet.)
mellissa
Thanku. I’ve just had an emergency op, and you hve given me some answers and sound so familiar to wht I’m going through now.
Lee Strausberg
Thanks for this article. I wish i had found it prior to surgery. My shock was bruising, muscle tightness and severe tenderness LATE the day after. Right when you think it’s all over the effects show up and the numbing medicine injected into the wound during surgery wears off.
I’m going to take your lead and write a similar guide with pictures and give it to my doctor to give to other patients.
My other complication was obesity which increases risk of delayed healing because of the obvious strain and because fat isn’t well nourished by blood vessels. NSAIDs also increase the risk for delayed healing as inflammation is a normal stage in wound healing so i elected to hold off on NSAIDs for as long as possible because i couldn’t instantly do anything about the obesity (45lbs).
Colace worked well for me to prevent constipation. I started that and beano prior to surgery to avoid gas and straining after surgery.
OK. The vicodin has me rambling so I’ll stop here. In short. Thanks.
freemyheart
I wanted to say thank you for posting this. Read it the night before my surgery last month and knew what to expect. The pillow suggestion was great advice. Kept my cat from jumping where he usually does. So yeah… thank you!
Linda
Thanks so much for this candid advice. My surgery is in 36 hours…. Ewwwww… not looking forward to being still, and in pain. Hope you are doing well, again, thank you!
Brit
Thank you. You hit the nail right on the spot. Thus is exactly how things are and I’m still in recovery. Day 5.
hhdsales2015
Was it easy for the doctor to tell it was a hernia? How soon did you have surgery once you found out? Are you 100% back to normal? Did you lose weight in a sense because you don’t have the bulge? I am in pain and 1000% know I have one but I’m scared to find out! Best of luck to you
Heather
Yes, it was easy. Basically, I could do half of a sit up ( a crunch, if you will) and a bulge would pop up out from just above my belly button. My primary care doctor had me lay on the table and do the aforementioned, and agreed it was a hernia. I saw the surgeon a week later, and was schedule for surgery two weeks after that (so 3 weeks between diagnosis and surgery). I have been able to build my core strength back up, which makes me feel less bloated. If you are in pain, don’t be scared to see the doc! I honestly wish I had gone (and was able to go) sooner and just get it done with! Good luck to you, hhdsales2015!
Allen
Thanks alot your most likely helping hundreds of people A year don’t sell your self short.how long has it been now and what state do you live in ?
stylinspice
I’m a 32 yr old healthy woman and I just had this surgery about 3 weeks ago. This blog is the ONLY site I’ve found that gives an accurate description of the recovery process. All the “medical” sites and even my doctors kept down playing the reality of the situation. Thank you so much for writing all of this and for posting pictures! It really helped me prepare emotionally and to validate my pain and feelings during the recovery process. I’m the type of person who never stops so it has really helped me to let things go while I heal.
chi
Found this very helpful as my daughter just had surgeryl! thanks
MaddyWaddy
Thank you sooooooo much for this. I go into hospital about a month from now. I reckon that knowing these things could occur after surgery will make them not seem as bad… if they do. Thanks again for sharing!!! Cheers from Australia. – Mad
Melvina
I hope you request no Mesh. It can be done and should be done.
MaddyWaddy
Hi Melvina. Thanks but why no mesh??? 🙂
Melvina
Because mesh has been known to cause problems in the body in the long run. I myself had hernia repair last year and he used mesh. Well, unfortunatey, im scheduled to have surgery this March to have it removed. Go to face book “hernia Mesh problems” you will be able to read the many hernia mesh horror stories. Also, goggle search Bruce Rosenburg. The medical desk provides doctors speaking out about the reasons mesh should never be used in the body.
MaddyWaddy
Thanks again, Melvina. I’m definitely looking into this further.
Cheers
M
MaddyWaddy
Okay. Since your message, I’ve done a bit of goggling on the matter and found this:
http://www.noinsurancesurgery.com/hernia/non-mesh-hernia-repair.htm#gsc.tab=0
and
http://www.noinsurancesurgery.com/hernia/open-letter-in-support-of-mesh-pain-patients.htm#gsc.tab=0
I’m going to do some thinking about this. Thanks for the heads up, Melvina. 🙂
Cheers
M
MaddyWaddy
Oops. It seems that leaving web addresses may not be allowed. Sorry about that. Please delete the post. It won’t happen again. Thanks. – M
Heather
Maddy it’s allowed! It’s simply that the blogging app requires me to approve comments with links for some reason, and I hadn’t been online since you left them. You should see them now 🙂
Melvina
Yes, i was able to see them. Im glad you’re doing research at least when you make your decision you will be educated on the differences. Most surgeons will make a person believe that they wont know if they can repair without mesh until they open the person up, saying it depends on how big the hernia is but thats just not true. I wish i knew all of this before i had the mesh repair. Im traveling to the noinsurance “Dr. Kevin C Petersen is actually doing my repair next month.
Ive had to phone conferences with him before ever meeting him, then i went to see him in person in Dec.2015. He gave me an exam, reviewed my previous CT scans and op report. Talked to me and didnt charge me dime for any of it. He was very personable and easy going. He never tried to push surgery on me. The 1st time i spoke with him in August 2015, he actually told me to give myself a few more months to make sure the pain wasnt because my body was still healing, i had just had my surgery in July. He said if im still experiencing the sharp glass cutting pain by October, to give him a call because i shouldnt still have pain by then. And i actually wanted to make sure and gave myself until Nov and then called back. My original surgeon insists the pain has nothing to do with the surgery. Which is ridiculous, its in my mid lower abdomen and it has been determined by 3 other surgeons that a tack is stuck to my body and that the mesh used is much larger than what was needed, and keeps me from being able to stand up straight without a severe pulling.
Im so glad for doctors like Dr. Kevin C Petersen who was referred to me by another surgeon from Tennesee who also removes mesh and repairs with no mesh. Both surgeons are recommended by other hernia mesh problem patients who had it removed. As well as Dr. Ramshaw from UCLA, but because so few surgeons remove and repair without mesh they have long waiting list for removal.
John Yanez
Day six and still can feel my hernia on one side (while just getting up or down, or walking). Hope my surgeon didn’t screw this up. Don’t want to go through it again.
Paul Panske
Thank you I just had it today. You are right…painful moving. Going to try the pillow. And yes I’m fearing pooping. So I found this, thanks again.
Craig
I am going in this Friday for the same thing you had done. Mine looks just like yours before surgery. I’m a little freaked out after reading your article. Should I be concerned? The surgeon told me it is relatively simple and I should recover without any issues.
Heather
I recovered without any issues Craig. Recovery was just a little harder than I expected. As in, I was down for about a week, uncomfortable for another week, then as good as new. Just keep in mind that it is invasive and you will be on the couch/bed for a few days. Other than that, it really is a simple procedure!
Craig
Hi Heather…thanks for the reply. Good to know. I appreciate it!
Michelle
Heather, did you experience an aching in your lower ribs and back during recovery? I’m thinking it is due to being bloated, but it’s hard to distinguish. I am now 9 days post op. I wake up in the morning feeling pretty good and as the day wears on I get more achy. Just hoping this is normal.
Jill Cummings
Michelle- experiencing the same. I’m on day 10 post op. I feel much better in am and as the day goes on I get more tired and achey. I had open mesh repair.
Renee
Thank you for posting this. There really isn’t a lot out there. Especially if you are a mom with diastasis recti. I’m going in for my surgery in March. How has the recovery been so far now that it has been a year? I’ve only had one baby but have to get this fixed before the next one. Thank you again. Great post!!
Melvina
If you’re considering mesh please visit facebook page “mesh problems ” or “fighters and survivors of transvaginal and hernia mesh” before doing so, it’s killing and, handicapping so many people. I myself am currently doing everything i can to have the mesh removed after my umbillical hernia mesh surgery last year. Ive been suffering every every since.
Courtney Smith
I know this blog and this comment was posted over 5 years ago but I just had my surgery done yesterday and I am so thankful that this blog and this comment exists. Why aren’t more people sharing their experience? Lol. It makes me want to write about it so others can have a good idea of what to expect. This article was perfect for me because, heather you and I seem like the same person (we both don’t like to sit still and I have had two babies too :))
Thank you so much for sharing your story. It relieved me and gave me so much hope to start my road to healing and recovery 🙂
And the momma who commented. I feel seen and I hope you do too!
Tina
I’m 7 days into my umbilical hernia repair (no mesh/non-larascopic). I am still in much pain and unable to walk around comfortably. I live an active lifestyle so this has been difficult. Reading this post helped me relax knowing another active person still experienced pain this far in. All other posts are medical and say the typical “3-4” days, which I do not think is accurate.
Thank you for sharing your experience.
Valerie
Thanks for sharing. I also tried to cut b ack on the meds too quickly and alds sticky realized that was a mistake, trying the icing now as the nurse at the hospital suggested that. I should have started yesterday but I was still groovy did not remember until today. I am a skater so also want to resume my activities soon but have been told to wait st least 4 weeks.
Shelley
I had surgery on the 5th of February . I had o growing hurnia & belliebutton hurnia. I’m still in pain I can’t sleep in my bed it hurts so bad I half to sleep in a recliner how long will this last ?they gave me hydros for pain and oxycdine for pain there not helping
Heather
Hi Shelley! I’m sorry you are in so much pain still. I would contact your surgeon ASAP. I personally was not in any pain after about a week. Good luck!
E M Turman
I wanted to say that I just had this repair done myself at the age of 45 by a remarkable surgeon and staff in Pinehurst. I will say thought it wasn’t a pain free experience it was a professional and true to life experience. I agree with everything you said, and the bathroom issue is no joke. It is rough. I had a hard time expelling the air from the surgery and still after day 3 am struggling. I tried the drug free method and that went to the way side after missing two doses. Never again. I too hate pain pills. I had tons of swelling in the groin area from the gas, and I can say that the sooner you start walking the better you feel. Thank you for the insight, I wished I would have read it before today. Good job documenting the process.
Thank you
ET
Dawn
Thank you for sharing your journey. My surgery is next week.
Elizabeth
Thanks for this honest first-hand experience. 5 days ago I had umbilical hernia surgery, but no mesh was necessary. I’ve had good days and bad. Weaning off the oxycodone. Not being able to poop has been the worst! Very frustrating! I’ve used Miralax, Ex Lax and an enema. Finally today I had some success! Still very bloated. Definitely look and fee pregnant. My post op appointment is this Monday. I sure do miss lifting weights in the gym.
Tracy Tienor
I need to get this procedure done? How long until you started lifting again?
John Yanez
Start walking as soon as possible, (probably after two or three days). I made the mistake of not moving much because of the pain. After 8 days I went back to the doctor because I was still in pain. He said get back to work (including a lot of lifting). I did that day and felt much better almost immediately.
anna armfield
Thanku for your helpful advise i am having the same surgery in a weeks time and il b sure to have a pillow as my new best friend
cathy
Did you get glued or stiches? How gross did your belly bottom get? Had my done Wednesday it looks really gross I was glued. No mesh I got lucky there thanks I so needed this
dh
I am on my ninth day of recovery.my first surgery ,I am almost 50 years old.you don’t realize how much you use your core until this.I still have pain but started using ibuprofen on 3rd day of recovery.my doctor is telling me no work for at least 5 more weeks.but I climb ladders ,lift & pull heavy weight on my job.I’m a truck driver but that’s part of my job to.guess I will have to get used to doing nothing for a little while longer.I thank God for my wife being the best nurse I could ever have.and I most of all thank God for comforting me & helping me through this.
Misty
This is exactly what I was looking for – I have the same surgery in about a month. Thanks for the great info!
Marci
Thank you for sharing your experience. I’m having the same surgery next week and was under the impression that it was a simple procedure and wasn’t that big of a deal. I’m grateful to know what to expect now since there is little information on the internet about it. My husband is now preparing for the week ahead. Plenty of microwave meals and taking care of me. Sounds great having me time except for the pain and boredom!
SKY
How long did the soreness last. I feel fine but still sore after 2 weeks
Robin Donahey
I found your story before having my own surgery on March 15th. I have to say that even though I have had 2 back fusion surgeries and some complicated hand surgery, your story made me very apprehensive. Now, I must also add that I have been Surgical Technologist/Surgical Assistant for 35 years, and I have participated in many of these surgeries. So with that said, I was still nervous.
My reason for having the surgery was because I had been suffering with bronchitis the entire month of February and the constant coughing affected my small umbilical hernia that I have had since having my children 26-30 yrs ago!
For all my apprehension, I am happy to report that i experoenced none of the problems you did after your surgrry. I had relatively minor pain, I slept in my own bed, no constipation, and my belly button looks better than it has in 30 years! At my 2 week follow up last Thursday, my surgeon said he wants me to do anything I want, except lifting more than 25 lbs.
It was a much better experience than I was anticipating since reading your story.
My word of advice for anyone who needs to have the procedure…
Every patient is different, experiences differ from patient to patient, so take these stories with a grain of salt.
We all have different medical histories, pain tolerances and other factors that affect how a patient responds to a surgical procedure.
Best of luck to all!
Marci
Robin, thank you so much for this comment. My surgery is scheduled on Friday of this week, April 8 and after reading many comments I have been a nervous wreck for the past few days after reading this. Now I feel so much better about the surgery knowing someone had a more pleasant experience than what I expected. Thanks so much for calming my nerves. I’ll update how my surgery went this weekend.
Michelle
Thank you. Reading these stories has made me very nervous,,, and I am hoping I do well with it. Did you have a smaller hernia? Mine is small, but I have been uncomfortable since November. They didn’t diagnose it as a hernia until recently or I would’ve had it taken care of by now!
Marta
Thank you so much for this article. I just had a surgery for 3 small hernia along my linia alba this morning, one of them was an umbilical one. I got very little information from my surgeon and I started looking for some tips online. Funny thing, I also have diastis recti (2.5 fingers) after giving birth to my son a year ago and I am also working as a personal trainer and class instructor. I will follow every single single tips I found here. I had an emergency C-section and I thought I was a super hero and went for a small walk on the fourth day after the surgery and after two weeks I was able to go fast and for long. I ended up having a very bad scar tissue. I will now take it really easy for a week like you suggested and so poo wily build my strength up 😉 One more time thank you
Brad
What does the belly button look like 4 months after i have somewhat of a inny but still looks like skin pulled together def not a full inny
Susan
Thank-you for posting this on your blog. I’m at 40 hours post-op (abdominal hernia repair), in a lot of pain and feeling very discouraged. I’m a runner and rower who’s really anxious about being side-lined for the next few weeks. Your blog-posts really help. Thank-you.
eric
Just wanted to say this was very helpful, I’m a personal trainer as well so this was perfect to stumble across.
Eileen
Thanks for this Heather. I’m planning my umbilical hernia surgery soon & your tips are greatly helpful!
Patty Nantell
Thank you for shearing your experience. I’ll have my done next month traditionally, not laparoscopically. I’m a nurse and I do A LOT of pulling and pushing, so it’s making me a bit nervous. I’m thinking about maybe taking about 3 weeks off. Do you think that’s realistic? I’d appreciate any thoughts on that. Thanks a lot!
Patty Nantell
Sorry for all the typos, autocorrect
Tracy
Heather, I am about to undergo the surgery to repair my umbilical hernia and they are going to close my diastasis (also two finger). I was wondering if you choose not to do that and if so, why? That might be too personal, but you being a personal trainer, I thought you may have some reason I’m unaware of.
melissa dragon
Hello. My name is Melissa. I had open umbilical surgery six days ago and feel this is kind of a slow process. I am a 33 yr old mom with a 14 year old son. I’ve had this hernia for awhile. I didnt have any mesh but they glued my incision, maybe because I’m allergic to adhesives in bandaids. I don’t know. Anyways, getting up from a laying position was hardest for me and the bowel movements. I am not currently taking any medications but trying to move around is helping me. I started getting kind of depressed and hated having people help me. But you have too. My appetite is good but should drink lots of fluids. I plan on going to work on day 8 but everyone keeps saying its too soon. Take it easy is the main thing and my Dr said I may need this don e again someday.
melissa dragon
Thank you for posting about your experience heather. I really felt Like reading this helped me feel a lot better. How long did you take off work? I’m a dental assistant and took off a week. Not sure that was long enough. Also, I took the dog out on a leash (18 lbs) yesterday and I shouldn’t have. People should definitely wait to walk their animals. Everyday gets better though.
Patty Nantell
Thank you for sharing your experience and your advice! I’ll have a mesh, and I’ll have plenty of help, my husband is taking a few days off plus my sister is coming from Topeka Kansas to help me as well (we’re Hispanics, we are super close, lol) I do have 2 dogs as well and I also have a dog sitter for them. But do you think 3 weeks is enough time? Like I said in my previous comment, I do a lot of pushing and pulling at work. I keep reading that a traditional incision repair may take up to 6 weeks to fully be back to your usual work activities. Your thoughts? Thanks!
Melissa Dragon
Patty, I would say if you can take the time off and can afford to, I would. I know you cannot lift over 10lbs for like 8 weeks but I’m sure every dr. is different. I have my follow up tomorrow so I will know more. Three weeks off sounds good then maybe just light duty for a few more weeks. Its been 6 days for me and I wish I could have just one more week. My boss though had a laproscopic hernia repair done but not umbilical, done on a Friday and was back to work on Monday! No recommended. Let everyone help you and maybe your family could make some nice meals for you. hehe Good luck with your surgery!
Patty Nantell
Awww! Thank you so much for your advice and kind words. Yes, I will follow your advice. My surgeon always is like “when do you want to go back to work” lol, he obviously tells me when he feels like I’m good to go back to work, however he always says “this is your body, tell me how you feel” especially with pain and lifting restrictions. My mother in law just signed up to help me too, she’s a saint! And my daughter now is coming home from Nebraska so that makes me very happy. What sort of activity do you think I should do post op to keep moving? Should I wait a couple of days? Or should I play it by ear? I’m sorry I’m asking so many questions!
John Yanez
I had a double hernia operation and my doctor used the mesh. He told me from the start I’d be as good as new and could lift whatever I wanted after a week. After 8 days I was still in a lot of pain (the pain meds were nearly useless) so I went back to the doctor. He told me I should have been up and moving around after 2 or 3 days and that I needed to get off my butt and back to work. He also said that with the mesh movement strengthen it. I was amazed to find that he was right. The more I worked the better I felt. Within a day I was almost back to normal.
Patty Nantell
That’s great to hear! What kind of lifting do you do at work? I pull and pushed a lot! I get a lot of bariatric patients that are total care. That’s my biggest concern
John Yanez
All kinds. I was lifting futon mattresses when I hurt myself. I was lifting things about 80lbs pretty quickly.
Simon
Wow, I’m having the surgery in two days and now I feel sick about it having read your story.
I too can’t sit still and it has haunted me for weeks, just the thought of not being able to move around.
Thanks all the same.
Johnny
Thank you for posting this. I had the surgery yesterday and im in a world of hurt. I wasnt expecting this pain. This was my first surgery as well. The process of laying down to standing is the worst. I’ll try the pillow.
Patty Nantell
Did you have it laparoscopically or open incision? I have my scheduled for May 20 with an open incision. I’ve had several surgeries, but I’m still apprehensive. Thanks
Sarah
Thanks very much for sharing your experience.
I’m on day 5 post surgery & I wish I had read your post before.
For me the severe bloating & constipation is the worst part of it. I think a stool softner or enema should be recommended from day 1. On day 3 I spent 5 hours in the worst pain trying to poop ! I felt like I was in labour again. Ugh.
I have a 7 month old baby at home & I think I should have waited as I’m still nursing & of course he needs my care so rest is not always possible for me. I have great help though & I couldn’t have done this without them.
Good luck to all in your recovery. We are stronger than we know !
Suz Smart
Hi ! I’m also at day 11 and have stumbled across your article as I google recovery post umbilical hernia as I’m dying to get out and run !!!
I’m training for my second marathon this year with a few halves and trail events in between and it’s killing me not being able to get out there !!
Thank you so much for writing this as I know that I’m also not yet right to run even though my surgeon said after a week or 2 I’ll be back on the road ! Every day it’s getting better and I can sleep on my side not just on my back …
Everything you wrote I was nodding my head , I’m at exactly the same place as you were when you wrote this !!
Xx suz
Amanda
Wow! I found this by googling. I just had mine done 5 days ago and holy moly. I needed so much help. I did not anticipate it being so sore and painful. I feel so much better but I look pregnant. Agh! Your info made me feel sooo much better. Glad there is hope for the swelling! Thank you!
MaddyWaddy
Hello again. Here’s my experience>>> Well, I had surgery yesterday (20 April). It went well. I had two small umbilical hernias repaired with mesh. I’m taking pain medication according to the box and thus far haven’t experienced anything too severe. The area is swollen as predicted. I do, on Heather’s suggestion, have my little pillow in tow as well. 🙂 I had my first loo visit this morning. It took a while for gravity to do its thing (as I couldn’t push) but voila. 🙂 I had already bought prune juice and had 1/2 glass with dinner last night then a glass of water. I’ve had another 1/2 glass with brekky this morning then a glass of water. From past experiences not associated with hernia, I’ve learned how to keep my system going to avoid constipation and also how to ‘do my business’ without pushing/straining. I slept pretty well last night and am up this morning walking around a bit. I’m moving very gingerly as I don’t want to do too much too quickly. I’ll report back in a few days to catch you up on my progress. Thanks Heather et al for sharing your experiences and offering advice. See ya. – MaddyWaddy
MaddyWaddy
Hi again. Today is Saturday — Day 10 after surgery. I’m happy to report that thus far, my time has been pretty breezy. Luckily, I haven’t had any of the serious bouts of pain I’ve been reading about on here. The surgeon removed the dressing during my 1-week follow-up visit the other day. He was happy with how the wound was healing. My navel is sticking out quite a bit and my tummy is swollen but that was expected-ish. I’ve been moving around from Day 1 and am walking outside heaps more/further every day. I’m not picking up much weight but am longing for the day I can return to the gym. 😉
I am sooooo happy that Heather and all of you have shared your experiences. They made me feel much better about everything. I mentioned this blog to my doctor as well, telling him that if it hadn’t been for this blog, I’d have been very scared with the swelling and such because he, THE DOCTOR, certainly didn’t tell me what to expect. All the best to those healing and those about to have the surgery. AND AGAIN — THANK YOU Heather!! 🙂
Cheers
MaddyWaddy Down Under
Joann mills
Thanks for posting with such honesty! I had a very similar experience. I am shocked at how much the doctors downplayed the recuperation.
Lucy
I have to say that after reading this blog & all the comments that I was pretty scared to have my umbilical hernia repaired. I nearly canceled a trip that was scheduled for 8 days post op, even though my doctor told me there was little chance I wouldn’t be able to fly. I am a 59 yo female in excellent shape, like the blog author is. I walk 40-50 miles per week and use hand weights for arm strength. My hernia repair was fast, just 14 minutes under anesthesia. I had an open incision like a half moon under my belly button. The doctor used two internal stitches and then surgical glue on my skin; no mesh. I want the readers here to know that this surgery is not necessarily awful. I am up and about. I walked two miles today, 24 hours after surgery. I was able to roll over in bed last night, sleep on my side, on my stomach, get myself in and out of bed without pain, walk, get dressed, etc. pretty easily during my first 24 hours. I am constipated from the anesthesia and am taking stool softeners that I expect to kick in eventually. Bearing down is not painful though. In fact, none of this is. I am sore, like I had stitches, that’s all. I was given 30, 2mg Dilaudid pills for pain. I took one when I got home yesterday afternoon, and another one eight hours later. I slept like a baby last night but my stomach was queasy this morning so I haven’t taken any today. I plan to take one tonight to put me to sleep, then I’ll be done with them. I took two Advil this morning & that got me through the day. Now it’s almost 10 PM & I’m sore & ouchy, but not in terrible pain. Ice has helped. I like the feel of the weight on my belly too. I am a little bit lightheaded, but I expect that to pass. Walking seems to help with the little pain that I have.
Lucy
48 hours post surgery update, well, it’s 55 hours post surgery – Still feeling well. The nausea is gone. My plumbing is working. I’ve been on a fresh fruit & vegie diet since a few days before surgery. I only ate saltines & spaghetti noodles with a little butter & salt on the day of surgery. Yesterday I ate a fruit smoothie in the morning that was a little much so I switched back to spaghetti noodles. The fruit made me a bit nauseous. Last night I ate a baked potato before my dilaudid & slept like a baby again. I walked 1.5 miles this morning then took a two hour nap. I’m going crazy watching bad TV & just took another walk, (it’s 6:30 PM now). My belly is sore & I’m going to ice it. I think my ridiculous fatigue is from the anesthesia. They gave me fentanyl, which the doctor said didn’t knock me out, so they gave me a little versed too. I can’t really complain much.
Adam Taylor
just had my gallbladder taken out and umbilical hernia repaired. i was not fortunate enough to get the mesh since combining it with the gallbladder made it a “dirty” surgery and the risk of infection is too great. I’m on day 4 of recovery. the gallbladder was nothing, i feel good about that bc i can now eat without getting sick to my stomach every time. but the hernia, i believe has come back thru the stitches holding it in. mine was about 1-2 fingers as well. probably due to the occasional coughing, and sneezing. sneezing is the absolute worst, it feels like my entire stomach is about to tear open on me. the pillow does help a lot!! hopefully I’m wrong, but the little budge thats back in my belly button says otherwise… looks like i may be going back under the knife and hopefully this time he will be able to put in the mesh. lucky for you tho, my dr only gave me 20 7.5 hydros and will not prescribe anything more bc of all the new laws and BS, even tho i was willing to turn the old meds back in to show i didn’t abuse them. so needless to say, I’m out of pain meds and suffering. thanks a lot Doc! had i known this wouldve been the case i would never have let someone cut me open
Michelle
Thanks so much for this. I am having the surgery in July. Originally I thought it shouldn’t be too big of a deal, but wow! I really didn’t expect to be laid up like that. I will take advice from others who have posted and have things ready ahead of time so that I can get the rest I need and be prepared. From what I remember reading I need to drink lots of fluids, take a stool softener, get rest but yet get up and walk, try to eat light meals so that my stomach won’t bloat more, ice quite a bit, etc., etc. I sure hope it goes well for me! Thanks again for this informational post!
Melvina
I hope you will not be getting mesh put inside your body, if you are please read about the many, many patience who are suffering due to have hernia mesh put in their bodies, the complications and the enormous difficulty finding someone to remove it.
Patty Nantell
Oh no! I’m getting a mesh put in!! My surgery is this Friday
Michelle
Please let us know how you do. I hope it goes well for you!
Patty Nantell
I sure will, thank you!
Melvina
Please, please go to facebook look for the hernia mesh problems page or mesh fighters and survivors and more. Hernia mesh patients and even surgeons are speaking on the dangers of hernia mesh in the body.
Michelle
He did not mention mesh……..just stitching closed. I have another appointment with him before the actual surgery so I will definitely verify that. Thank you!
Tracy gamblin
Hi , I am three days post supra umbilical hernia repair via open incision ….friggin it is painful ,can only take paracetomol and codeine as get asthma . Also scared that one in twenty can happen again . How is yours . The thought of doing this again is too much to cope with . If I lay down for a while it’s the only pain free time ….u use your core for so much , I haven’t attempted going to toilet , think the pain will make me faint . This op is for brave folk and I am not ha xxxxx Tracy
Lucy
I’m so sorry that your recovery is painful, Tracy. It sounds as if we had the same surgery. I’m on my fifth day post op. I did not get mesh, did you? Mine does not hurt. I took two pain pills on the day of surgery & one the next day & then was fine with Advil for another day or two & that was that. I went back to work today. I can’t explain why two people with the same surgery have such different experiences with pain. I have a small half moon incision under my belly button & two internal stitches to close the hernia, which was above my belly button, then skin glue & steri strips. Perhaps yours was larger? Ice helped me, and walking did too. Walking helped stretch the area & also got my insides going. So did stool softeners, fruits, vegies & prunes. Check your wound to see if it’s red & hot. Infections are supposed to be very painful. Please keep us posted.
Michelle
Lucy, thank you for this. I go in for my surgery in July and I am SO scared! I am hoping I have a good experience and feel quite a bit better in a few days, but one just doesn’t know. I will take your advice and use ice and walk, along with using a stool softener and eating fruits and veggies. I am taking notes now so that I will hopefully have a decent recovery. Lucy, did you swell a lot? If so, how long did that last? I think that is one thing that can contribute to the pain too. I have a smaller hernia so I am hoping that means a little better recovery but who knows??? Thanks again for this post.
Michelle
Tracy, I’m so sorry you are still experiencing pain. I go in for mine in July, and let me tell you, I am not very brave either! I really hope you feel better soon!
Charlene
Thanks so much for this very helpful post! I am on day 2 of my recovery from non-mesh repair surgery and doing great. I’m a healthy, fit 58 year-old mother of 3, grandmother (!) of 2 who has lifted weights my whole life. So far, recovery has been relatively easy. Using a gel ice-pack has been helpful, along with lots of rest. Eating lots of fiber (I’m vegan) and drinking lots of water took care of the constipation concern. Finally got to remove the bandage and take a look at my incision today. There is swelling around the area that will hopefully go down soon. Looks like my belly-button has returned to its former non-outie state. I hope the remainder of my recovery goes as smoothly as the first 2 days have!
Michelle
Thanks for this! Charlene, have you been taking pain meds? I wonder why some people have a lot of pain and others aren’t so bad. I go in for mine in July and am hoping to heal like you are. I plan to do lots of fiber as well, along with liquids to avoid constipation. From what I have been reading that is extremely important to do with this type of surgery. Have you been up walking as well? Thanks again for posting!
Patty Nantell
Post op day 3. Pain not too bad, splinting incision with pillow. Taking ibuprofen and tramadol for pain. I’m vegan so lots of fiber and water, going to the bathroom has been a lot easier. I had a mesh put in and have dermabond on my incision. It is sligjtly bruised, i am now sleeping on the couch as the bed is too hard to get out off. I went into respiratory distress post extubation so they had to keep me overnight.
Steven McLean
Thanks for posting this very helpful blog and also to the many people who have responded with their own experiences which I also find very helpful. I had open surgery yesterday and am now on day 1 of recovery. The pain is excruciating but thanks to everyone here .. I now know that there is a light at the end of the very dark tunnel.
David
Hiya, David , 65 , retired , over 65s Masters Squash player
7 days post op to the minute ..12.15am UK.
I’m amazed at how closely my op has followed the “pattern” of recovery.
I started Googling the op because I felt that things were not happening as quickly as they should and that maybe I had done something wrong and torn internal stitches or something.
The wound has stayed clean and is healing well outside. Belly still very swollen and I was worried about the pot bellied look. It’s a bit uneven and more swollen on the right side.
Inside feels “jaggy” and although I think I could do better with my movement my brain is telling me wriggle into upright from sitting and use whatever solid supports are there for my arms and legs to avoid core movement.
Only managed one night in bed so far …. Lying flat feels uncomfortable and sleeping in a chair with leg support or on a sofa is much better.
Been driving and that’s OK although I know I shouldn’t yet.
Mowed the lawn a couple of times and lots of non lifting jobs around the house.
Am desperate to start training for my sport again .. Still at least 6 weeks away .. Grrrrr
Will take a long time to get fitness and skill levels back.
Have decided to break the recovery time midway with a sunshine holiday.
Cheers
David
David Ramage
Oh yeah, David again,
Also a former runner until lateral release operation (knee problem) ended that career in 1984.
Times are slow by today’s club runners but back then 3h18mwas a decent marathon for a 13.5 stone runner … (Did it “by accident” .. Started the day as a spectator and fellow club runner had stomach problem and gave me his number.
1h.21m best half marathon , 36m for 10k , and 4m.55s for a grass track 1500m
1h 25m in 1984 Great North Run got me into the first 800 over the line out of 25,000.
Mayra
Hi! My name is Mayra. I had an umbilical hernia surgery 3 weeks ago along with the removal of my gall bladder. Prior to my surgery I was very active as well. I know it’s over a year since your surgery and I just wanted to know, how much time did you take to recover before starting to run, lift weights, etc?? I know for me it’s still a bit early, but did you have any complications after you began working out? Also when I start… Do you think wearing like a abdominal brace would be a good idea? Please reach out to me since I just need advice before going back to working out. Thank you!!
Heather
Hi Mayra! I think this post might be helpful in answering some of your questions regarding my return to exercise! https://relentlessforwardcommotion.com/2015/07/umbilical-hernia-surgery-6-month-update/ As far as the abdominal brace, I think it wouldn’t necessarily be a BAD idea. If nothing else, it would probably give you more confidence to get back in the gym. Just make sure it doesn’t make you OVERCONFIDENT in that you push too hard, too soon! Good luck!
Hilton share
Thanks that helps a lot ,what about the actual site covered by a plaster to stop any moisture getting to the wound ,how long before this can be removed?
Robin .
This was all great information. Thanks for sharing your experience.
Steve
I’m a 33 year old male in good condition. 5’8 155 lbs. I’ve had 2 prior surgery’s an open umbilical and left inguinal at the same time.(no mesh in either) Then 5 years later another open left inguinal with mesh and a mesh plug. Now on may 11 I had a laparoscopic umbilical w/o mesh and right inguinal with mesh. Let me say maybe because of the mesh = 3 1/2 hour surgery. Woke up in excruciating pain. Worse than both opens put together. I thought it was gonna be a piece of cake. Wrong. I was useless. Could only stand hunched over. Could not get out of bed or even try. Couch or lazy boy is where to be. Ice and more pain meds than they said is what helped. And the doc did down play it. It took about 1 week to take less meds and 2 weeks to move pretty good definitely hurts when I twist or use my abs. I took stool softener (doubled up actually) but it didn’t work so I had to use milk of magnesia with that I went a day later but with grumbles and pressure pain. Don’t eat alot until you are passing unless you really want a stomach ache too. Be walk around. be active And it heals with less pain in the end. In my opinion. Then the scars will be more flexible. Pillows are key. Especially with seat belts. Hope everyone’s goes better than mine and I wish I found this post before my surgery lots of great and interesting info!!!!! Happy Healing
Melanie
Is it normal to have a very swollen belly after umbilical hernia? I feel like i m pregnant. I did surgery two days ago!
Carine
This nails exactly what I’m going through. Didn’t think it would be this last after having tubes tied did nothing. Boy was I wrong!
The odd thing is that the incision are on my left side (laparoscopic) but it’s my right side that hurts. Feels like someone has me by the guts when I try and move. I’m also having to close my eyes and mentally focus on using legs and arms ONLY and leaving core completely relaxed….not a single twitch of muscle movement
Kathy
Hi…hope u continue to heal….I’m on day 9 and can relate to everything u said…I’m doin well but at a slow pace which is not in my vocabulary but I want this to b a success
Thanx for sharing….I’m not gonna lift anything 4 a,while lol
Jill
Great article. I am day 4 post op and you are spot on with everything. I have two children -7y.o and 5y.o and I was not not the extent of the impact on daily life/pain. Glad to hear it’s all normal
David Specht
I weighed about 197 lbs before surgery and 207 lbs after. Is this to be expected?
Heather
Hi David. I imagine there is probably some swelling and water retention due to the trauma of surgery that would show up as weight gain on a scale. TO be honest, I don’t own a scale, so I don’t know if this happened to me. But when in doubt, always ask your physician!
Michelle
I haven’t had my surgery yet, but I would think that would be from swelling. How long has it been since surgery, and have you been icing at all?
Laura
When you were in recovery did the Dr have you wear a ab binder, I’m 5 days post and still very swollen.
Heather
No ab binder for me. I was swollen for quite sometime as well. But as always, if you have concerns, talk to your physician just to make sure this is a natural part of the healing process!
Patty Nantell
He didn’t but I’m doing it, it has made a huge difference!!
Clare
Hi there, thanks for your blog! Helped a lot!
I have my operation in a few weeks time, I’m going on holiday 3 weeks later, do you think that this will be enough recovery time ?
Regards
Clare
Patty Nantell
Cannot post more than a couple of sentences here, email me at [email protected]
David
This is a good read!! I am four days post op but everything you wrote about in this is spot on, literally!!! This ” no big deal” surgery as they call it, is a ” pretty big deal”!!
Michelle
David, what are you personally finding is helping the most? Are you still on pain meds? Do you have bad swelling?
Michelle
Do/did you prefer MiraLax or Colace as a stool softener for starting before the surgery? I am trying to be on top of the game and want to have something on hand. Someone had mentioned to me to have Milk of Magnesia on hand for after the surgery as well. Any thoughts?
Chic Scaparo
Holy cow Heather I’d swear that I wrote this article haha. I’m glad I found this as I’m experiencing the same exact recovery as you. Athletic, can’t sit still, and in day five of recovery — it’s been brutal! I was reading this to my finacé who actually asked if I wrote it. I completely stopped the meds after day two and a half and only take a couple of Aleve for sleeping at night; I’ll take the pain over the opioid daze and the bathroom issues 🙂
I was curious when you were able to run again? I’m going a little crazy and need to sweat.
Thanks for the post, Heather. It’s helped me make sense of what the docs or nurses never mentioned.
Michelle
You sound like one tough cookie! Thank you so very much for this blog article. My husband who Never goes to the doctor has to have the same surgery in the morning and I’ve been researching and by chance I found this and am very very thankful. He is bound and determined to be back at work in less than a week, he has never taken more than 2 Advil, and isn’t much for help. It’s been a whirlwind as the doctor got him set up with a surgeon and surgery within 2 weeks. Everyone keeps telling him how common it is. I like to prepare and you have eased my stressed mind and I thank you very much. On a hunch (thinking about how I felt after giving birth) I bought him a cheap body pillow but other than that I could not think of what to do for him. I now am glad you mentioned the ice packs and I will have a family member grab some mirilax as I cannot imagine that pain. Once again Thank You & I just hope that you are back to the active lifestyle you had before the surgery.
One less stressed wife,
Michelle
jess
Thank you for this. I am currently 4 days post op and I struggle mostly with resting. I had the laparoscopic procedure and it’s very painful. It fills you up with gas that causes a lot of pain as it passes around. I have 3 children (ages 10, 2 and 8 months). I don’t like not putting them to bed or being the one to get them up in the morning. I too refuse narcotics and still have not taken any other than when I awoke from surgery. It made me high and that’s it. I’m stubborn about sitting still as well and I’ve been paying for it since surgery. I’ve had 3 sections classic incisions and none have hurt this bad. But I’m finally giving up in trying to do it all and finally taking it easy before I end up with another hernia. Thank you for this, I now know what I’m experiencing is “normal”.
Don
Great information! Stinks when you’re single and have no one to help 🙁
Ruth
WOW!! I just went through this surgery on 6/20/2016 and WISH I had googled this topic before now. I was a little too nervous to go on-line at the risk of seeing or reading something scary.
I have been having a very similar experience to you. In lieu of mesh however, my surgeon opted to try using stiches to correct the issue as he felt it was small enough.
I am a group exercise instructor, and I am very active. The size (I think……mine was two finger tips) and location of my hernia was the same. Your #s 1, 2, 3, 5, 6 and 7 are word for word my experience. I was laughing and shaking my head at the same time, for not finding this sooner. How I wish I had not tried to be a hero on day 2 and shun my meds like you did!
I thought I would be back at work the next day, made it through one day of work (I think post-surgery meds and adrenaline) and then paid for it for the next two days. Day 3, I caved and went back to taking my meds and booked day 3 and 4 off of work too. I buckled down and tried to mostly sleep my way through the pain. You are right, I thought “out-patient surgery can’t be that big of a deal, I’ll be fine!”
I am now on day 9. I feel fine and have almost all movement back. Only a little discomfort once in a while. I was told by my surgeon between 8 – 10 weeks before I should go back to my active lifestyle!!!!! This is driving me nuts!!!! I know I shouldn’t push it, but how long before you felt like you were ready to start back up again, and how long did it take you to get back to your pre surgery lifting weights/distance/times?
THANK YOU so much for writing this.
Anyone reading this who has not yet had this surgery, learn from this article, it was too similar to my experience for words!
Rachel Felt
Thank you for your post! I am also a personal trainer and very active (workouts, mom of a toddler, ext). I am laying in bed, 9 hours post-op from my own hernia surgery. This helped calmed my nerves a lot! Thank you for the tips and for sharing your personal story.
Courtney
Thank you for your article. I just had this done 6 days ago and was trying to see if the swelling was normal as I too looked 4 months pregnant and wasn’t warned about it. Do you have any new pictures? My stomach looks similar, just wondering what it will look like months/year later. Thanks
Ruthy
I know this is an old post… but thanks for making me feel i am not alone!! I am currently in bed recovering and wow this is worst than a csection and i have had two!!.. i had the hernia repair plus got my tubes pressed at the same time.. idk if it makes the pain worst buy i am in really bi pain… yes taking my pain killers ar a must!!.. havent pooped yet and i am scared to lol… i just had the surgery done 18 hrs ago…
Michelle
Thank you for this! And thank you to all of you who posted with helpful hints! I had my surgery July 14th, so I am on the 4th day of recovery today. This has been pretty much spot on for me. I found that the pain meds made me too constipated (along with the anesthesia) so I chose to only take them through the morning of the second day. I went with Motrin after that. What has helped me the most has been doing lighter meals, eating fruits and veggies, taking stool softeners twice a day, walking starting on the second day (a little farther each day), and icing with gel packs. Today I can honestly say I feel as if I am turning the corner. I do notice when I tend to overdo it, and it is frustrating not to be able to do what I want. I went to two grad parties three days after my surgery, and it was too much too soon. So just know if you’re going through this to make sure you plan to have a week of “nothing” going on. One minute I can feel decent and the next I am sore. Last night I still had a hard time getting out of bed to use the bathroom. We will see how tonight goes. It helps to sleep on a couch or bed that isn’t real high up for a while.
Brooke
this helped me tremendously with my recovery! Thank you! I am 3 weeks post surgery and I have a pulling feeling on the lower right side, which is the opposite side of my incisions. Anyone know how long this will last or if this is normal? I had 2 hernias, umbilical and the one above it repaired with mesh.
Michelle
Did you have an aching in your rib and back area throughout recovery? I am experiencing that now.
Richard Davies
Hello I had just had umbilical and inguinal hernias together two days ago. Your comments above give great advice especially about the popping something that is a worry right now . Thanks for the help good to read about the actual experience. Hope to update later
Richard
Taisha
Hello Everyone –
Thank you to Michelle and everyone who has replied! I had my umbilical hernia removed yesterday. I’m about 28 hours postop. I have been reading this thread and other blogs about recovery. Most have been horrendous. I’m glad I didn’t chicken out as I did two years ago to correct this. This hernia and Diastasis Recti began after I gave birth to my three year old daughter. The bulge changes in size and is not very nice to look at. Anywho I believe I spooked myself but I don’t want to speak to soon because although it has been a lot of discomfort the pain is manageable. The hardest part is picking myself up out of bed to use the bathroom. I have been drinking vitamin water and water consistently along with taking 5mg hydrocodone, colace and miralax to curb constipation. This is my first surgery ever (29 y/o female fairly active walker/ 3 miles a day) I can’t wait to recover because I was offered a new job and I don’t want to miss the opportunity due to recovery. I want to add that my uvula is hanging low and that is more painful than I thought it would be. The breathing tube really irritated me.
I hope my recovery doesn’t regress but so far I can’t say that I’m in excruciating pain. Just a lot of discomfort.
Michelle
So glad it’s over for you! Yes, getting out of bed was the hardest part for me too! I am on my 11th day postop today, and I feel pretty decent for the most part. I went to a party yesterday and sat for a long time-came home a little swollen and sore-but mostly I feel pretty well. I just can’t overdo or I do end up getting achy. So……..I do things in moderation. Things will get done in time I guess! Each day gets better-glad it’s behind you!
Jami Studer
Thank you for this!!! I’m getting this surgery on Friday. I have two kids. I’m worried about picking my daughter up and straining something. I, too, am very active. When did you resume non-core working out??
Lindsay
This is a great post. I’m 5 weeks post surgery. I have laparoscopic umbilical hernia repair. I’m back to spinning classes and going hard and don’t feel any pain in my core, however, when I try and do sit ups or TRX resistance and I’m focusing on abs the top area of muscle under my ribs, still feels painful. Like a burning sharp pain. It’s tough to push through it. Any recommentions for this or any idea when this will get better?
Thanks so much!
Jami
How long before you started working out again? I’m still pretty sore just walking around, and trying to walk around with a straight back! I’m 4 days out.
Sheenagh McManus
Fabulous article xx I’m 4 and 1/2 weeks post op umbilical hernia, open surgery repaired with sutures… Has anyone else noticed a small bean size link… I’ve got one where hernia was it’s extremely painful…gp says he thinks it’s,a build up if blood.. does anyone know how long this would take to go.??? Any advice is greatly appreciated
Di
Thank you! Super glad you shared your experience & that I found it.
Ayansmom
I just had hernia repair with Diastasis Recti tightening exactly a week ago and my belly looks so hideous now. I look pregnant and there’s a bug egg shaped lump at incision sight. I did not have mesh btw. I am hoping this belly goes down and this lump decreases as well. I would’ve lived with my hernia and DR had I know how ugly it’d look after. Hopefully it goes back to normal soon.
Wendy
Thanks for sharing I had my hernia surgery 7/18/16 only area that’s sore is my navel!! Think belly binder stay on to long. Calling doc tomorrow!!
Michelle
Is it continuously sore? I had mine 7/14/16, and I do get little pains in my navel every so often still. Not buckle down pain, just a little pain here and there. I’m assuming that is normal unless it were to be continuous? I haven’t done anything overly strenuous as of yet so I would think I wouldn’t be agitating it.
Mike
This describes my experience almost identically except the pillows on the arm of he chair. Wish I thought of that I was leaning too much into it. I’m on my 6th day and only stopped the oxy last night as I’m not a fan of pills unless absolutely necessary. Help is essential, like you said “bet you didn’t realize how much you use your core” WOW! Things I’d never even think of, it’s almost like not using your thumb. I get out of bed in steps and literally coach myself through it. Thank you for sharing your experience on here. I’m going to check out your 6 month recovery article, my goal is to get back into the gym and be able to sit-ups until I collapse with no worries. Hope all is well with you now. Take care
Kylie Carberry
Thank you for your great information on umblical hernia repair! I am on day 2 post surgery and not too bad. It’s been super helpful to read your progress as the doctor didn’t really say that much about how long it would take for pain and swelling to ease. Thanks again!
Bob
Hard the surgury Wednesday, stopped the pain killers today friday found no difference after I stopped the tylenol 3’s, only have pain when getting up or sitting down, so might as well try and avoid the constipation, mine was a small hernia so maybe that’s why I’m not suffering as much as some here. Trying to do some small walks during the day, there is some discomfort but not to hard to take, pre surgery the anithesologist told me I had a really good surgeon he had done his hernia, think I lucked out….
Jennifer Melville Mccrossin
Your story was very helpful as i am very swollen , i am 45 years old & a busy rescue mom i have a ranch full of horses & 3 kids , i am at day 3 recovery , after going in my dr found it to be bigger than expected requiring 2 more hours , i also had double breast augmentation due to loss of most of my right breast 2 months earlier , right now the hernia area is where im feelig the most pain & swelling ,witch hazel has been great at soothing pain & swelling , and hooking my hands under my knees to get out of bed is the only way i can get up , my dr sent me with a velcro wrap to support my stomach close to your pillow 🙂 thanks for sharing !
anita
I just had this surgery yesterday and reading this post and your experience makes me feel so much better. In fact so much so that it sounds like me…. I too am a runner/athlete and sitting still is not something I am good at. However, this pain sucks and is real and I thought I was being a wimp before reading your story. Thank you for putting me at ease and for sharing this.
Anders
Thanks for the article! My experience is a bit different, though. I had the procedure (traditional incision without mesh) done, here in Sweden, 5 days ago. I’m a 35 year old man who visits the gym and swimming pool every week, but not as much as you. Still, the surgery didn’t affect me much. I walked home afterwards (even though they urged me to order a cab), and after having rested for a couple hours I returned to my office. The next morning, I could bike to a meeting with my client without any problem.
I have a prescription for two kinds of painkillers, but as the wound doesn’t bother me I haven’t picked them up. Of course, it hurts when I sneeze, or when I get out of bed or a couch, but I’d rather have those reminders that I’m doing something that’s potentially harmful. In fact, my experience is so different from what I was prepared for that I had to call the hospital and ask them if something is wrong with me, but they assured me that it’ll be fine and that I don’t have to take painkillers if I’m not in pain. Yesterday, the wound started to itch. That’s a bit annoying, but I think I’ll manage without pills.
I guess I’m either lucky, had a great surgeon, or simply a minor hernia to begin with.
Mario defoy
Thanks for your story. Just had the procedure 5 days ago. Still painful like a burning sensasion with swolen stomach.
Will use icepack tonight like you suggested. Hard for a busy guy like me to watch netflix allday… But now i believe in crop circles, know hitler fake his suicide and escape to Argentina untî the 1970s and rewatched all the classic movies that gives up my age; top gun, forrest gump and rocky,123 and 4 lol.
Anyway, not do easy surgery, dont do anything at all except watch tv or read in bed for a good 5 days. I walked and drove my car a little bit after day 2 and i think i am suffering extra for it now. Thanks to you and to the internet for the info. Mario montreal canada sep 05 2016
John
I really appreciate your sharing this! I just had the surgery done yesterday and it was my first ever surgery so thank you for helping to alleviate some of my fears on the second day. I truly appreciate it!
Annie
Thanks for sharing this. I’m scheduled to have an umbilical hernia fixed in the next 2 weeks. Not really looking forward to the recovery but these are helpful tips!
Maria
Thank you so much for sharing your personal experience! I just had my hernia repair this Wednesday so about to hit 48 hours post op. Your personality and habits are a lot like mine and was not prepared or expected this much pain and swelling! I really thought I was going to be in minimal pain and walking about much more. Boy was o wrong :(. I have had 3 abdominal surgeries but I will tell you this has been the most painful!
I also too look like I am 4 months pregnant. Tummy is firm, tight and incredibly tender with any movement; deep breathing, coughing even talking. Every little move is painful. Besides the medications, ice ice And more ice provides so much relief!
I am also an athlete and cannot sit still! At 35 I am having a hard time resting and staying in bed. Trying to take it easy especially since I have been on my own since I was 19 and never had someone there to help me out. I now have an amazing significant other who has been so supportive and wonderful about wanting to help, but I have a habit of not asking for help because I feel bad. I have to get over that and ask for help when I need it. I believe you pointed that out, which is very true and glad you mentioned it.
When were you able to get out of the house and go to the store and run errands? I have been up and about around the house in small increments to keep my circulation flowing. I haven’t gone #2 yet so I started taking a laxative but nothing yet! Passing gas but that’s all! I wonder if I can take benefiber or something of that source to help aid the laxative but I will call my doctor.
Again thank you for sharing your experience because I was beginning to think something wasn’t right with the firmness and amount of swelling and pain I am having. I will be also following up with my surgeon next week just to be sure there is no infection or anything of that sort.
How many weeks post op are you?…. And how long after surgery did your swelling and pain go down? When can you start running again?
I hope your recovery is going smoothly and you are feeling back to normal soon!
Mary-Louise
Thanks so much for writing this. I’m on day 7 post-op for my umbilical hernia repair and and a regular hill runner and Ashtanga yoga practitioner. So am champing at the bit to get back to normal bit don’t want to do too much too soon! When did you get back to running?
Sarah Elliott
Brilliant to read something that actually means something to me. No medical jargon just how it is. I had para umbilical hernia repair open surgery only 4 days ago and boy do I feel like poop. Wandering if it’s normal to feel like I do cannot get up or poop you have summed it all up for me and actually made me feel a lot better that it is normal to feel like this thanks for your honest comments I think I’ve got quite a way to go yet and like you I do not like sitting around from a very sore Sarah x
Rajan
Beware of constipation – add fiber, kiwicrush juice, probiotic yoghurt, water ; laughing & coughing pains the most (im still in 1st week post op umblical open cut surgery – mesh); dont be surprised on how much core engages when lying down or getting up from bed, causing pain. Day 5 & definitely feels better!
Monica Medina
Wow this really helped me I have been searching for others that have gone through this.I’m also an athlete and it’s so hard to just lay around.thank you so much for this information.
Pg
I don’t normally write on these things online but I really want to say thank you for writing this. I am looking after my 15 year old son who had the operation yesterday. Like you the doctors gave very little indication as to how you are affected post op. He too has requested sleeping on the sofa for the same reasons as you. He tried the pillow on the tummy and that brought relief too. He too worries about needing to go to the loo and we also decided to keep to small meals and highish fiber food. He was feeling quite down and shocked about how debilitating the operation is until he read your post. He recognized everything you said and he understands much better now. You have helped me help him. Thanks for taking the time.
Pamela Smith
Just one word to all you future undergoers of this surgery: Kefir. I am now on day 11 of my recovery from open surgery w/mesh to repair my umbilical hernia and I did not have one single problem with pooping after the procedure, unlike after past surgical procedures where I would be miserable for days because of constipation. This time I was given full anesthesia and oxycodone for pain.
I started taking Kefir about a month before the procedure – about 2 oz. every other day or so — and was blown away by how “regular” it helped me become. That was the first good news. Secondly, I can now report that using it ALSO resulted in no constipation AT ALL after surgery.
You can thank me later.
Bri
Omg!!! I feel like you just read my mind!! I had ventral hernia repair surgery 2 weeks ago today! I’m a VERY active person! I have a full gym in my home which I use at least 6 days a weeks, 3 kids 8 & under. Just had my 1st check up after surgery today and I started crying in the office. The dr was like “are you ok”! Inside I was screaming “noooo” I now he said 6 weeks but 2 weeks feels like a life time! I too have never had surgery besides wisdom teeth. All three kids were vaginal births. So this is all shocking to me! 2 weeks later and I STILL look 3 months pregnant!! is this normal? I was told today at Drs office it would go down, but it’s freaking me out not being able to work out! Not eating too much bc when I do it hurts feeling full. Is this all normal?will I ever get back to normal? Can I get a flat stomach ever again?? Believe it or not after 3 kids I did have one, minus the hernia bulge. Thank you for posting this! I’m so happy I found this post tonight bc it calmed me a bit!! Thank you!!!
Sonny E
Hi all! Am 70 y/o male, retiree. Had my open umbilical hernia op last Friday, September the 30th. Thank heaven everything went well. I will consider myself very lucky/happy since I did not have any problem after the surgery up until now. Just rested fully, took a lot of fluids, applied ice 24-48 hours. I didn’t have to take any pain med. Hoping I can drive now, will see my surgeon next Friday, the 14th. Thanks to my Florence Nightingale (RN) wife, my recovery is going fast pace. Wishing everybody well!
Glenn Condrey
Just had the surgery 3 days ago. I also have never had surgery other than wisdom teeth and like you I hate taking pills. Just had a physical 3 months ago and in excellent health. I’m a very physical person who does not like sitting still and at 60 years old my mind thinks I’m 40. Thanks to a wonderful girlfriend of 20 years who made me follow the postop instructions I’m feeling much better after the 3rd day. Although she wanted me to sleep in the bed i was more comfortable sleeping on the lazy boy couch where I could prop my feet up and every 4 hours take my pain killers and walk around inside the house. I now have no pain while in the lazy boy but still have slight pain about a 3 when getting up and walking around not planning on going back to work till after follow up next week and then only if doc says it’s ok as work is a lot of lifting and straining. My point is to people having this”SURGERY”. Don’t be a tuff person. Be a sissy and listen to the doc and follow the instructions
Cevan L. Cross-Hall
Thanks for sharing your experience! I am a very active person also, six days at the gym with two or three days running each week, and I have the same surgery in two days. Its nice to know what I can realistically expect with similar circumstances. Thanks again!
Christina
Hi,
I similarly, have two kids, am a runner, and had an open umbilical hernia repair and only found one other personal story online (male, which was sort of helpful, but it’s nice to get a female perspective!). Thank you for posting your story. It was incredibly encouraging to read your post and see your pictures and know even sort of what to expect. (Found it the day before my surgery.)
My surgeon decided the day of my surgery to do it without mesh. While they were in, they found a muscle tear which they also sutured. 🙂 All of your suggestions were spot-on. I highly encourage the ice to anyone reading – it was particularly helpful in recovering quickly. I don’t know if you had this – but the only strange thing I’ve had post-op is that I get cold really easily! (I’m two weeks post-op today.)
Thank you again! Hope you are doing well!!
Brandee Nephew
Thank you for sharing! I am a runner & have been running for about 4yrs now. Nothing over a 1/2 marathon yet, & I faithfully go to the gym. I also lift on a 45lb child through out the day as part of my job. I thought I was in decent shape! It’s been a month since my repair & it’s feels like I’m starting all over again! My runs feel like they did after having my daughter! My digestive system is a mess & my stomach still is pretty bloated. I know things could be a lot worse! I’m not asking for sympathy just advice? I’m not a quitter so I’ll keep going till I’m back were I was.
Eri
Oh wow thank you very very much for this post. I am on day #4 post op and I had to (sadly) erase my marathon training for this year because of this hiccup. As I was reading through your post, I couldn’t stop but to nod and agree with each point you made!!!
Claire Casey
Thank you so much for your blog it was just what I needed after my operation, it was so hard trying to find any info even from the medical team.
Thank you from Claire xxx
Jacqui
Yes I had the same experience. Absolute agony in hosp for one night on codeine and paracetamol. I needed morphine. I managed to get up onto the commode in absolute pain on my right side as if my hip had been punched. The next few days I had swelling and terrible backache due to lying in my back on bed. I couldn’t turn over at all. I got a hot water bottle for my back and felt so much relief. I felt sickly at times and felt very sleepy. I also had a bowel movement on 5th day after taking senna. It’s so hard not being able to use the core as it just won’t work. I’m resting more now and taking ibuprofen. Still bloated up. Hope to have 3 weeks off work or 4. It’s incredibly painful the 1st 2 days so keyhole is no easy ride.
Kaykay
I’m glad I ran into this post I just had the same surgery two days ago and my doc said the same thing 48 to 72 hours I would be fine NOT!! IM still in so much pain and u r right I tried sleeping in the bed last night won’t do that again worst sleep ever. I was really getting concerned about my post surgery pain until I read this..thank you so much for this personal post!
Carolyn
Thanks for sharing your experience. As a competitive runner, mother of two and recent (2 days ago) receiver of umbilical surgery I can relate to many of your “mistakes” (stopping your meds) and trials. I am experiencing what I think is heartburn but may be abdominal bruising or something like it. Glad to hear my stomach won’t look like this after a week. Looking forward to being able to jump out of bed in the morning and walk a few steps without abdominal pain.
Philip
I had a similar experience to this. I had surgery 8 days ago, and feeling a lot better than the day after. I am a very active person involved in intensive training for sports, and thought I would be out for 6-8 weeks, but at this pace, I think I could start training again in the next two weeks. I stopped taking OxyContin after 2 days, and weaned myself of Ibuprofen 2 days ago. Post op in 2 days!
Fadzai Takarinda
Thank you so much for this. My procedure is in a few weeks and this article has really helped me to prepare.
Andrea
Hi! Thank you so much for writting this, as you I will be facing same surgery next Friday and wanted to hear personal ‘tips’. One of my biggest concerns is how soon could I be able to be back to the gym and if at least I could be able to walk in the treadmill. Also I was also hoping to be fully recovered after three weeks to be back to working out my abds. I would.love to hear from your personal experience now that time has passed how was the end of your recovery.
Michael
I think what you said helped.I had it done last week and the pain is still really bad.Did you have mesh put IN?
David Tapp
Many thanks for the very helpful articles.
As far as I’ve seen, and that’s a lot of surfing, yours is the most helpful website on the web, for detailed, well-laid-out, first-hand experience of a mesh repair and of umbilical surgery in general.
I’m having exactly this procedure next week and I wasn’t stressing because I’ve had many surgeries for various injuries. However, it has been really useful to have a blow by blow account of this whole thing.
I opted for a mesh repair as I’m planning to be working my core pretty hard, as a rock climber.
Tragy
I am 4 days post-op from same surgery and I still found this helpful!! Thank you for posting this!!
Question for you….
Did you have really odd grumblings and bowel sounds post-op? I am, and it’s weird!
Gemma Ridgway
I would like to let you know you post has really helped me! Im day 3 post umbilical hernia repair and its so nice to read something so honest and accurate. I also can’t believe how incapacitated I feel right now. And oh my god you’re so right…who knew you used your core this much!! I know this was written a long time ago but reading it has helped me to see light at the end of the tunnel. Just wanted to say thank you! 🙂 x
Jodi
So happy to find this post in my searches. I too am a fellow athlete and not one to sit still – this is already “killing me” and I haven’t even seen the surgeon yet. Thanks for sharing your experience!!
Mayeli
Thank u for the tips. I just had umbilical surgery and it sucks! Finally I found a good blog that is helping me understand why it’s important to REST.
Chris Weston
Because I underestimated the procedure, I’m sitting here trying to find out why I still hurt so much 6 days after a dual hernia operation- the inguinal hernia op is nothing- but the umbilical hernia recovery is really causing consistent discomfort and 24 hour soreness and stomach distention. Your story describes exactly what is happening to me. Well written and the most honest appraisal I’ve come across. I didn’t see the doctor after the op although I had one overnight in the hospital and I won’t see him until at least 3 weeks have passed. Because its over Christmas and doctors need their holidays too. I took my dressing off and it looked so horrible (you know!) so I quickly put another one on.
I don’t like taking too many pain killers like yourself and I’m about to go and try your suggestion of a cold pack. I’m male and 69 years old. Thanks again for writing what you did. I’ll live!
Angela
Thank you for this! You’re right – there’s hardly any personal accounts on line. All I’ve found talk about how common this is in elderly, obese smokers…but like you, I’m young and highly active. I was starting to feel broken! My surgery was just yesterday, so I feel like I found your post just in time.
Elle Bee
Thank you, thank you, and thank you again for candidly sharing your experience for others (like me) to have an idea on what to expect. Like you, I’ve only had surgery for wisdom teeth (20 years ago!).
Roxanne Goodrich
Hi. You site has been so helpful, and all the posts have been wonderful.
I had my umbilical hernia operation on January 3, 2017. I see it’s been a long time since anyone has left a comment. I, too, have a Diastasis from having an 11 pound baby. 4 fingers. I left my hernia go for about 10 years – but it wasn’t the hernia that got me into surgery – it was an emergency appendectomy. I had the appendectomy performed laparoscopically, and the surgeon pulled out the appendix close to the hernia so I didn’t have mesh to repair the hernia. Nut, the fascia around the hernia was so frail,and in such bad shape (from waiting so long) that I have to be very careful. I am day 5 post-op. I came home with a 12″ compression belt which the surgeon says I will wear for at least 3 months. Like most, I haven’t yet had a bowel movement and am afraid to have one for fear of blowing out my stitches! I am bloated beyond belief, gained 10 pounds. (fluids?) and am still in a lot of pain at the hernia site. Very discouraged.
Heather
This post was very helpful! I have my umbilical hernia repair surgery on Wednesday Jan 11 (1.5 days!) and am very nervous about it. I tend to get over-anxious about these kinds of things. Thanks for all the post-surgery tips, I will definitely use them for a smoother recovery. What did you wear to surgery and post surgery that was the most comfortable? Do they make you get into a gown for surgery? Also, any tips on staying calm when they start to put you under?..
Thanks again! -Heather
Joseph
I am 67 years old male and I had umbilical and ventrical hernia surgeries on 01/05/17. Sedation was used in my case which I am gratful for.I was told post surgery that all went well and I was discharged less than two hours after the intervention. Pain was significant only the first two days, then subsided gradually after that. I took half a Percocet during the first two days every six hours, and did not need any medicine after that. Today is a week since my surgery, and I have been able to walk a couple miles a day on my trademill for the last three days (approved by surgeon) with marginal discomfort. I expected the whole ordeal to be more painful, now I realize that my worries were unfounded.
kirsty
Thankyou for the insight although slightly apprehensive about my hernia surgery next month. Like yourself I am a mum of 2 and I work and go to the gym at least twice a week and like to keep myself fit and healthy so this is worrying me as I am not one to sit around and I am worried ill never have a trim stomach again??
Amanda
I know your pain I also had my gallbladder taken out too along with this umbilical hernia surgery I am in so much pain and my pain meds aren’t helping that much.. I have a 6 month old who’s 19 lbs luckily I have a bug family that’s helping me. I’m still in the 24 hours of this ,. I can’t wait to feel better!
Amanda
I meant big .. autocorrect…
ColoradoMom
Thanks for sharing! After reading your blogs about her surgery experience I am nervous. My doctor has reccommended surgery for me as soon as possible, but I have a newborn, 1 year old and 3 year old- all who still need held and picked up. The Dr. Made surgery sound like no big deal so we had planned to do it this spring, but I’m curious what your thoughts would be. Should I consider waiting a few years? Currently I have no pain with my hernia, it just looks like an outie. I really can’t afford to be “out of commission” (unable to pick these babes up) for multiple weeks. I appreciate your thoughts!
Full-time employee and mom of 3 under 3!
bella donna
Hi. My mum is 82 and she had op like you. She is concerned because the op has left her with high blood pressure and swollen feet. The nurse left her on intrevenous drugs for too long and a machine preventing blood clots pumped almost 12hrs may have something to do with her swollen feet. Unsure. Plz comment.
Anita Faulkner
I am 63, not an athlete, and having umbilical hernia surgery next week. This will be my third surgery in less than a year (multi-level lumbar fusion and fractured hip repair). I also have a numb left foot and leg and am walker-dependent. Because of that, I have difficulty getting up from my sofa. I have a lift recliner. Do you think I would be comfortable sleeping in that during my recovery from the hernia surgery? Thank you so much for sharing your experience.
Mike
Thank u for sharing that is very sweet of you.
Melony
When did you discover your hernia? I am 4 months post partum and I discovered my hernia about 3 weeks ago. It is pretty uncomfortable, but I just don’t see how I am going to be able to recover when I have a 16 lb baby to care for. I am also a very active person so having to back off of my regular workout routine because of my diastasis recti and umbilical hernia is driving me crazy.
Doreen
Ty for this article! I just had the surgery…no way 3 days! I am in so much pain, and the pooping thing is just horrific! Have had 3 children and gall bladder surgery, this is the worse by far! 2 days post op….
Shilo
5 days post open navel hernia with mesh. I appreciate you all sharing your stories of recovery as this helps me prep for what may come. I pulled myself of all meds by end of day two. I don’t have the intensity of the stinging pain much. However I have a lot of pulling. I find that I wake full of energy feeling and feel like today’s the day I’m going to accomplish something. By late day I’m sore, my back is tender and I end up calling it a day by about 5 p.m.
Looking forward to some normalcy again. Doc says give it 8 weeks…
Erin Thornton
I wanted to say thank you so much for this information! You have made my day. I am, also, an athlete, wife, mother-of-two, and about to have umbilical hernia repair surgery. I am terrified of not being able to do anything active. I have never been able to sit around, and this scares me. But, I need to have this hernia fixed, as my youngest is now 7….it’s time. You have been honest and given me more details and information than anyone else has (even my doctor). Thank you so much.
sarah
Thank you for this article! I was searching “umbilical hernia surgery” for my husband, who is two days out from the operation. Maybe you should go back and edit out the funny parts. He found yet another thing we use our core for when he laughed.
Rick Garrett
I have a question for anyone that has gone through this recovery. Did the Doctor give you any pain meds and/or antibiotics to take during your recovery? I had this surgery at a V.A. hospital in Muskogee, OK last Thursday. I believed it went well because I was discharged later that day and sent home to recover. I slept the rest of the day awaking Friday morning around 10:00 AM. The pain was at about a level 10. I then realized that I was not given any pain bills for my recovery, nor was I given any Antibiotics to help against any infection. The only thing that I was equipped with was a support, velcro wrap that stretched around my waist. When we took this wrap off (because it was itching terribly) we realized that they had not even dressed the wound and my stomach had broken out in a rash do to the wrap. I was in tremendous pain with no pain meds, no antibiotics, no “true” dressing over the wound and an allergic reaction to the support wrap that I was given. Is this Normal? Do Doctors usually preform surgery on a person, through a support wrap on them, and them send them on their way? I’m just looking for some answers because I have a feeling that the Doctor that performed my surgery really didn’t care what happened to me after I left the hospital. In other words I feel as though I was treated as a number and no one cared if I was Okay or not.
Michelle
I was given a script for pain meds, which I took up until day two because I didn’t like how they made me feel. Plus I was constipated on them. After that I just took Motrin. I was not given an elastic wrap but they did dress the incision. I just kept icing it every so often which helped tremendously. (Gel ice packs). I was given an antibiotic in the hospital before the surgery in case of infection and showered with antibacterial soap before going to the hospital. I definitely think you should’ve been given an option to take pain meds. Not everyone takes them but the option should be there. Also, it seems odd to me that they didn’t put a bandage on the actual incision. I hope all goes well and that you heal fast considering it all.
Sharlene
One thing that was not mentioned here is the horrific pain the gas they put in your abdomen during surgery causes. Besides the awful shoulder pain gas bubbles move around and get stuck in your ribs and under your sternum. My surgery was awful – throwing up, problems with bowels working, gas bubbles in my abdomen and intestines. Took me two weeks to get back to work and 4 weeks in I am still having pains and I do believe the hernia has come back as a result of projectile vomiting. Worst surgery ever.
Keri
Thank you so much for a great article that was well written I too am active lift weights run and bike and was wondering about recovery and when I can get slowly back to working out and being active has not quite been 24 hours since surgery very painful the second day the initial getting out of bed was the worst thinking I might sleep on the couch in in the recliner section
Karen
Thank you for sharing you story, my husband just had the same surgery yesterday. Did you have to wear a brace home? He has one and he says it’s been feeling so tight. Also I wanted to ask you when you started eating and what did you eat in the first few days following your surgery? He’s only been on clear liquids since he’s been home and I don’t know when or what to start feeding him and he’s hungry, different websites I’ve researched have reported different things. So confused now.
Abril
I really hope I haved found this post sooner … I try to have help but it back fire and haved me helping take care of 5 sick kids instead of my regular well rested baby’s … I could not carry them but first week little sleep and not much rest cAn leave you with lots of pain and baby’s to breast feed so no more hard meds and have to keep going at your 120% when you feel like 30% recover .
Amanda Pendley
I’m sooo glad I found this post. I’m scheduling my own umbilical hernia later this week. I’m a runner too so I’ve been pretty nervous about it wrecking my workouts. Thank you so much for sharing your experience!
Deb
Thanks it really helped me the pain is pretty nasty wasnt expecting that i had 2 unbilical hernia s repaired 3 rd day on and no better yet, maybe because im older 54? And over weight doesnt help ? I dno but truelly didnt think it would be like this
Deb
Steven Williams
I had the operation 16 days ago it is still not healing it keeps on weeping of blood and don’t no what to do. I have been to the doctors and gave me some tablets to take but not working.
Julie Philippe
Omg I’m on day two and in lots and lots of pain….. reality of what I read rings very true right now and I’m yet to use the toilet ….. scared and hugging my pillow… this sucks!
ashley
Hello I had my surgery Friday and bit is now Tuesday I was wondering when will I be able to sit up from a laying down postion without wincing in pain?
Larry Becht
Hey would you mind if I emailed you. I’m just about 28 years old and would love to follow up on your hernia repair. I just had one done today and I am dreading the inactivity pain later on. My email is [email protected]
Arta Zvirgzda
Thank you for sharing your experience. I am on day 5 after small operation. I am really glad I read this article BEFORE the operation as similarly my surgeon had told me its not a big deal. I feel that the worst days are gone and I am getting better day by day (slowly). The worst thing was to get out of bed which was too high in hospital. My tip for those who are just planning the operation – dont go home the same day as in hospital there is 24/h care and you get good painkilllers (there is no option to recovery without them). Good luck! ☺
Manda
I have trouble understanding what I can and can’t do. I made a mistake the first day wasn’t thinking. And moved the couch a little so I could lie down n watch tv. I’m to use to doing things for my self I didn’t even think to ask. Then I shock a plastic bag cause I thought she asked me to make the bed I got yelled at again n she said she don’t think I know how serious this really is. Of course I know how serious it is I didn’t think shaking a garbage bag was that bad. Now I’m not loud to leave the bed only to go to the loo
kylesmitsdorff
I’m reading this because I just had the same procedure done last week tuesday. I had never had any form of surgery and this was a big deal to me. I had an umbilical hernia for about 17 years which was small and I was able to push it in and it would go away and then re appear if I coughed. I was concerned about it potentially getting bigger so decided to consult with a surgeon.
The surgery was scheduled for the next day and I was able to leave the hospital about 2 hours after the procedure. Its a week later and I had the dressing removed by the physician yesterday who said that everything was ok.
I dont know if this is in my head but I can still feel the bump. Its not as visible as it once was but I am bloated like someone who is 11 months pregnant and i just feel really disappointed. I used to be able to push this thing in and now I cant, I can feel it if i put my finger into my belly button and lift up. Its clearly there. Dr says its scar tissue but I know what it used to feel like. Is it normal to still have a bump a week later? Could it be swelling or just scar tissue and will it go away.
I had such high hopes for this procedure and now im just miserable. My back hurts, I cant walk up right, going to the toilet is really hard, I cant drive. Im just annoyed. Dr assured me yesterday that there is very little chance of it coming back but I dont know.
WIll make another appointment with him and see.
Anders
I was in a similar situation as you, when I had my surgery in the end of August of 2016. In my case, the pain was minimal and I never needed any painkillers, but I was worried that something was wrong and went back to the hospital for a check. They assured me that everything was better than fine, but I still wasn’t convinced. I had pus coming out of the wound, suture thread from the abdominal wall piercing the skin, a belly button that was still bloated, etc. I was disappointed.
Despite all my concerns, everything turned out fine after a couple of months. I’m now going to the gym four or five times a week, plus running and swimming, but nevertheless my hernia hasn’t returned. All that you can see now is a scar that’s slowly fading. What’s most surprising is that although I’d been ashamed of my belly button for as long as I can remember and never wanted to go to the beach, my self-esteem about my body has now completely changed. I had imagined that, having never been happy about my belly in my life, this would require serious work, but somehow my brain just immediately accepted this “radical” modification to my body.
Hopefully, your experiences in a few months will be as positive as mine. I wish you the best of luck!
Natalie Phillips
I’m also a second timer umbilical hernia surgery patient, but for some reason this second time around is different. Today i became scared when I say the entire area around my naval swollen. I got a litlle sign of relief when i read your experience.
Wendi
Thank you for sharing, I’m sorry that you have to go through that again. Your atorh is claiming my nerves because next Tuesday I am having surgery for the same thing umbilical herina. My doctor is doing an open ventral hernia repair and I’m freaking out!! So reading about what you went through is comforting to know and easing mind for recovery. So thank you to much! And good luck on surgery number 2.
Monica
Thank you so much for sharing your story. It helps me have a better idea of what to expect in a week.
kathy
thank -you for your help /my surgery is tues 7-11-17
Nathalie
Interesting to read this as it is hard to remember to take it easy and let yourself heal. I had the same procedure 5 days ago. It has not been sore. The orangey colour around the navel is the same. I was tired for the first three days, but have found not being allowed to drive the biggest hassle. My tummy makes me look pregnant and it was reassuring to read that you had the same problem. The most important thing to organise for me was someone else cooking dinner the first few days and school drop off and pick ups. I felt a bit teary from the anesthetic and have been a bit grumpy and have less tolerance with my 6 kids. I am spending today organising some play dates for next week.
Thanks for sharing your story, Nathalie.
Louis
Makes me not want to have my surgery but if I don’t the results could be deadly. No pain No gain.
Shelley
I had my sergery about 3 mounths ago now and i felt fine at first healing at what i thought was at a normal rate but one day i got out of bed like always very carefully n bam it hit me this very sharp intence pain like burning sharp pulling like stiches were sticking into me inside its not healing n im worried i went to doc and she said give it a mounth n then we may give you a scan or something im not happy. I cant move even a little even sitting hurts whats wrong with me ???????????
Heather
Shelley this happened to me as well. A good friend who is in the medical field told me what I was feeling was likely scar tissue breaking up. When I finally went back to the gym, I had about 24 hours of that burning as well, and then it went away. If it doesn’t go away, I’d definitely recommend going back to your doctor!
Patti-Ann Gracia
Hi Shelly how are you feeling now. I had my surgery 1 wk tomorrow. My stomach hurt at first on the left side then acouple days later it was hurting alot inside on the left and then all over the stomach but weird not in the belly button area. It still hurts horribley to lean forward or to get up off a chair. It feels like my stomach has something in the way and wont fold the skin. Then on the out side my skin is very sensitive and even my clothing or me touching it it feels like it is burning. Does this sound at all like you are or have gone thru? If I just sit here i don’t feel much but if I touch it or more oh its not fun. I still have had to take pain meds daily. How long did it take for these symptoms to finally back off? This surgery is a lot more than I ever thought it would be and I have had many surgeries this one has not been fun at all. Debating if I should call my Dr or hold out. Thanks for your thoughts.
Patti-Ann Gracia
I know its been 2 yrs for you now but f you can still see these comment. Please tell me if your 1st wk you had tearing pains in your whole stomach and your shin felt like it was burning when anything touched it including clothing. It still hurst to bend forward like my stomach won’t fold like it always did if that makes sense. This is all a’lot more than I thought it was going to be. Its been 1 wk since my surgery. 🙁
Clari
Thank you for to sharing this our story! I just had hernia repair surgery and DID not expect recovery to be like this and found comfort in your story, so thank you 🙂
Talent
I just had a umbilical henia operation.
It is painful can’t deny that but my worry now is that it’s now 10 days and I still feel pain and changing sides during the night is a lot of work because I canot just turn as I used to.
My worst problem is sitting down, in a space of 20 mins I will be in pain. I have to take double dosage of pain meds.
Le
I am 51 and have just had umbilical hernia surgery and have had multiple major surgeries in the past. This has by far been the most painful even worse than a hip replacement! Am on the 4th day and still in extreme pain and unable to do anything on my own. Your blog speaks the truth. I have no idea why any doctor would say only a couple of days of pain. This surgery has totally “put me down”!
[email protected]
I just had this surgery today and found your article very helpful and honest. Thank you!
Poonam
Hi I have been operated since a week now but still feel the pinching pain and today could see the purple spots around the stitches . Can u tell me wht it is ?
Amelia Vitale
Reading this next to my husband who has been out of surgery for about an hour. This reassures us both on the next couple of weeks. He is also very active so sitting still could be the hardest part!
Trevor h
My Surgeon and GP no doubt have more info than they have passed on to me re post op hernia experiences . I am 48 hours post op for the 2 hernias in question, l am still in pain but not at yesterday’s level, the bloat under the bottom of my left rib cage is causing most discomfit. I am advised tomorrow I can start driving again? So far the constipation problem has not occurred ((good portions ‘ of water and fibre ) !
I’m not sure what you meant in reference to core strength , l have good core strength, is that bad?
Right now I feel good, but no matter how I feel during the next 12 days I’m going to continue to bore myself silly and hopefully get through with minimal pain
Catherine
Hi there. Great article. I have undergone an umbilical mesh hernia operation and 11 days later have this huge swelling just above the belli button. It is painful to the touch. Is this normal as I am concerned that the hernia looks worse than before the operation.
Michelle
Truly thank u for this! I’m 6 days post op from the same exact surgery. Mine was caused by my hysterectomy 6 months ago! Surgical incisional site. I read through your first surgery and was shocked when I read u woke up pain free! I got to the end and saw u wrote the hernia returned and just screamed “NOOOOOO!!!” Then when I read through your second surgery, I said, “ahhhhh yes. That’s just like mine! They placed the mesh on top of your hernia in the first surgery. They TACKED the mesh underneath with the laparoscopic surgery. I was told THAT is the way you wanna do it. Mine was huge. I’m a bodybuilder/manage a gym and so fitness prob was the reason it got so big. I’m sad, my powerlifting days are over. I hope u have since recovered from the second surgery!
Pedro Jr.
Thank you for sharing your story. I am back home sitting on my favorite chair with my feet up on the Ottoman. Got home about an hour ago from the hospital. Everything went well thank GOD. You were so right regarding general information. Your insight and personal experience give an idea of what to expect. You covered all the bases. I will continue to read as I see you had to have a second surgery. Mine was like your but two repairs and two mesh’s had to be used. You explain everything do well.
Thank you so much your writing is appreciated and very helpful.
P. Acosta Jr.
Singer
Thank you for such a good review – Im day 4 of emergency surgery (same procedure as you) and am 5 months pregnant. I also thought recovery would be a day or two and I would be walking ok but that is not the case at all. I have absolutely terrible bloating and discomfort after eating and I am not eating much. Pain has dropped off however tenderness when walking is still not easily tolerable or standing upright.
Im glad you posted this as it seems each surgeon who advises ‘a few days and you will be back at work’ hasn’t gone through it!
Natera
Thank you this helped out so much as i was concerned about a few things!! ❤️
claudia chavez
did your belly botton have a strange odor?
Steph
I had umbilical surgery yesterday and couldn’t be happier to read this ‘normal’ personal experience. I am in so much pain and wondered if this was normal after a few friends told me I’d be fine and back to myself pretty much straight after! Oh no! I don’t think this will be the case! The pain is indescribable at the mo but I’m controlling it with meds and my husband is my utter life saver and doing everything for me as well as helping me just simply get up and sit back down!
Thank you for writing your post x
Angela Flynt
I just had surgery yesterday it was open umbilical hernia repair with no mesh. Everytime I love today it feels like something tearing in my belly button. Is this normal
belen tijerina
Did you lose weight during the recovery and or feel a difference after the swelling went down? I have my surgery in 4 days!
Ronnie Stone
So how are you doing now after hernia surgery? Mine comes up in a few weeks.
Ronnie Stone
So how are you doing after your hernia surgery? Mine is coming up in a few weeks.
Shasta
I had my surgery on January 23rd.. And I didn’t eat for a whole week well maybe a Jello a day.. I was afraid to use the bathroom.. It was hard enough to wipe after I went pee but when my first bowl movement came I screamed in horrible pain.. I was not shown the proper way to wipe myself growing up so wiping hurt so bad when I had to bend forward.. And I’m a heavy person.. My pain is still here.. It hurts to lay down and it hurts to bend and sneeze.. Bowel movements today are not as bad.. Earlier I had to bend over to grab something and I screamed so loud and started to cry.. I literally had to sit down to calm down.. The hernia was the size of a melon.. The surgeon said it was really deep and they had complications on getting it to close because of scar tissue from past c sections and he also said something about my bowels being a problem.. I had the robotic surgery done and it went from a 45mins-1hour surgery to almost 3 hours in surgery and recovery was 2 hours.. I woke up screaming and crying.. They tried 3 different medications in my IV and the third injection calmed my pain down.. They didn’t keep me over night and I wish they would have and the only help at home was my two boys ages 7 and 11.. It was rough.. A little better now but still hurting when I walk 5 mins or longer and hurts to stand up for long periods and bending and sneezing hurt really bad as well.. I’m still on pain meds but don’t like to be dependant on them.. I had mesh and stitches but they said the stichtes would dissolve.. And the surgeon said its expected to be in pain still considering the size of the hernia and he gave me 3 more weeks of expected healing.. I’m just trying to figure out.. When I bend why does it feel like something is stabbing me in my stomach 🙁
Amy
Thank you for this detailed account of your experience! I’m getting my surgery tomorrow…
Jennifer
Thank you so much for sharing your experience. What you wrote helped me more than anything else I found on the internet.
Mary kangas
Just had hurnia operation. Thanks for the tips. I’m in week 3 of recovery.
Mike Mc
My problem is a little different from those I’ve seen. Need 2 inguinal hernias and a navel hernia repaired. My problem: Live alone on second floor. Nobody available to help. Am 69 and both knees are bad so mobility is limited. How long until I am able to go up and down stairs? Even if I have health aids and food delivered, I must use stairs to answer door. Can I DEMAND and extra day’s stay in the hospital? I am located in NYC. Having difficulty finding transportation home from hospital.
Heather
Hi Mike! To be honest with you, I have no idea if you can demand an extra days stay. It may depend on the hospital, how busy they are, etc. They might suggest a rehabilitation center vs. staying in the hospital (I bet it’s significantly cheaper too!) I live on a third floor apartment and had to walk up the stairs just hours after surgery to get home. Granted, I had a handful of people helping me keep my balance. Either way, I would highly suggest discussing your concerns with your surgeon. I’m sure that you aren’t the first to have these logistics difficulties, and they might have helpful suggestions. I hope you are able to figure something out! I wish you the best of luck!
william
I go in tomorrow. Will let you know. Have a small hernia so hopefully my recover will be faster.
Oxycodone does not work for me.
Ashley Hoeffler
Thanks for sharing, I’m on day #5 of recovery and my belly is huge! Doctor didn’t really tell me anything other than my restrictions of no more than 10# for 2 weeks then no more than 25# for 4 weeks more…
Mike
Your a wind bag dude, just get to the point instead of writing a book on your surgery.
Heather
1) It’s “you’re”, not “your”.
2) I’m a female, not a dude
3) This is a blog, not a medical site. The whole point is to write a story.
Thanks for reading though (I think?)
william
Had surgery at Bryn Mawr Hospital two weeks this Thursday. I had little pain after operation and needed no meds. Operated on at 9:30 walked out to parking lot well over a hundred yards at 2 p.m. with no problem.
Some discomfort. They gave me a percocet as I walked. Out.
Had coughing and sneezing that caused little discomfort in the lower abdomen .
I iced down for two days the first nite with a huge water chest ice pack, Had no swelling.
Having the best docs has to be part of it. Was in the fifth day back to my normal schedule. Told to rest a lot first 4 days.
Only problem is with fatigue. Doc said that would continue for 4 weeks and get better every day.
Saw doc on l0th day. Doc said things looked great. No heavy lifting till after 4th week. At this point can do lite weights, exercise, bike riding and stop if it starts to pain.
I guess I have been lucky. Ate raisin bran every day that helps with the flow of things. Had no constipation
and not problem going to bathroom. At lite for 4 days but a couple chicken cutlets.
Orderly told me to expect some belching and gas from the air trapped inside my stomach. Did not have laproscopic. Wasn’t the largest hernia but by the time of the op it was one inch wide and one inch high
which had doubled inside in two weeks when the surgery was planned.
I just want the fatigue to go away, but have been active walking almost 3 miles every day after the fourth day.
Had no bloating whatsoever so maybe the huge ice pack helped that. In fact, my stomach was immediately smaller after the surgery and lost two pounds right after getting home.
gretchen
Thanks for this. Very helpful! I just had this procedure and am curious did you use an ab binder? Did you ice the skin directly or thru that?
Heather
Hi Gretchen! I did wear a binder after the second surgery, not the first. It was given to me in the hospital to help reduce swelling. DEFINITELY a huge help in moving around and staying comfortable! I iced both direct and through the binder.
Porsh
Thank you for writing this.. about to have the same surgery in 48 hours and this really helped.
james f. vogel
THANK YOU. NICE SHARE.
Ruth
Thanks usefull suggestions
Laury S.
Am so glad I found your blog. The pictures have been a great help. This is the fourth day from surgery and I feel good but won’t push the lifting and straining due to your advice.
Thank you for posting this.
Roxanne Pynn
Thank you for this! I’m post op day 6 today and still so bloated! When did that settle for you? Same surgery but because it was a repeat hernia due my diastasis recti (i haf 2 kids as well but my youngest is almost 11) surgeon said he was going to sew it together too but it was just a small area. I was in the best shape of my life going into surgery and cant stand how inactive this recovery is but i get it so am listening to my body. I’m getting a little discouraged at how uncomfortable I still am and bloated despite taking it so so easy. Thank you again.
Zanab
Thank you! No one mentioned the swelling or applying ice. I was freaking out about how big I got!!!! Now I feel better. Thanks so much again!
Jennifer D
I wish I would have found your post sooner! I am 7 days post lap umbilical hernia repair and your article is spot on! It had some great tips that would have been good to know sooner! Looking forward to day 11ish when hopefully I will be feeling 90% better too!
MandaLynn Sudberry
Thanks so much for writing this!!! I had the surgery myself this last week and you helped me so much!!! I am 4 days post surgery and VERY TIRED, SWOLLEN, & Sore. But it’s gotten a little better day by day . Have a Blessed Day & Thank-You AGAIN!
Jenny Nigro
Thank you for this article! I just found out I have the same thing and im terrified, I love my stomach and hate that outta of all places…. I have to get surgery there….I have two kids and I am hoping my family will be helpful!
Eric
I had my surgery done on a Monday.. it is now Wednesday.. I too am very active and gym oriented.. I was truly unaware of the severity of this procedure.. I am a bit salty on how this was described to me as a “ couple of days” process.. it’s only day two and I am in complete agony.. thank you for your experience.. I would call it accurate and comforting as well. Thank You
Rhonda
I am on day 5 post op for the same surgery. Same procedure except when my surgeon was in there he found a second hernia higher than the umbilical and fixed that also. I also have mesh plus he sewed my muscles back together over the top of that. I am so glad for your post as I was beginning to think I was a giant baby. This hurts a lot and when it isn’t the pain of the muscles or incision it is the pressure making it difficult to catch your breath and extreme fatigue. I am getting better daily but still can’t sit or stand for more than an hour without having to lay down with pillows for support. I am off the oxy due to nausea but ibuprofen seems to be at least taking the edge off. One thing i would note is that I get muscle spasms in my abdomen which are painful and those occur randomly but also if I shiver when cold or start having anxiety. This may be due to the muscle sewing or the fact that I am not very athletic and have a desk job. Still not back to work yet. Hoping i can do some work from home later this week. I’ve had 3 kids and other surgery but this takes the cake. Key is to not push it at all. Glad I have plenty of helpers.
Sarah
I have just had this and I am in so much pain ,tummy looks like I am 6 months gone starting to regret having it done ,can’t go to the toilet everything you have mentioned .how long did it take you in the end to recovery fully I am normally so active tennis twice a week ,zumber pt sessions s many thanks Sarah
Elizabeth Tribley
Thank you for sharing! My son just had surgery, and was looking for some straight answers!
Carol Dobrowolski
I had this surgery Friday and was glad I read your account of the surgery. It was very helpful. I am a diabetic and pee about 15 times a day so I am always having to get up. For the constipation I took metamucil and stool softner. Took a while to kick in so I took peppermint essential oil and put 10 drops of it in the toilet and then sat on the toilet for about 10 minutes. Presto…it works. Also I use an elevated toilet seat I had for my total knee replacement. That has been a lifesaver!.
Louise J Milano
This really helped. At an active 86, I was thinking no big thing. But it is. Thank you.
Lindsay
Thank you for writing this. Thank you so, so much. I’m a professional athlete/mom who is one week post-op from an umbilical hernia repair and have really been struggling with recovery. I thought this procedure would be minor and I’d be back to normal quickly. Instead I’m still hugely swollen, pretty sore, and unable to exercise. It was such a relief to read about your experience and tips. I nearly cried with relief! Thank you!
Chris
Thank you for sharing your story. I go in for one in a few weeks. It’s small, yet I’m sure the shock to my system will be there also. How long did it take you to be able to drive again? Thanks
Pedro Duran
I’m on day 5 and have a burning pain still I’d call it a (6)
It’s not constant comes and goes thru out the day,just wondering if you felt a burn pain at all.. thanks…
Maya
Not sure if you remember since it’s been a while, but I just got the same surgery. On day 5. Relatively pain free besides when I overdue it. However, I still see a bulge where the hernia once was. Did you have that too? It’s freaking me out that maybe it didn’t heal properly or something! Post op appointment is in 9 days but found your page as a googled “what if’s”. Thanks!
Stacey Boyens
Thanks for the tips! All your information was right on and comparable to my own personal experience.
Stephb
This is day 2 for me, surgery was yesterday 5/3 at 9:30am. I have crazy swelling and was starting to freak out… sounds like that is perfectly normal now after reading your experience. I’m also scared to death to go to the bathroom! Thank you for writing such a straight forward article about post op hernia recovery! Wish me luck!!
Glyn
Thanks for sharing your experience. I recently noticed a small balloon looking bump above my navel but paid little attention although it felt soft and “different”. Next appointment, I asked my PC doc if it looked like a hernia and he said, ‘Looks like the start of one, might keep an eye on it but it’s small enough that it should be easily repaired.
I’ve had two friends with hernia surgery and they both had opposite experiences. One good, one not so much.
Now, after reading your experience, I’m not so sure. How long can I wait? Does it enlarge quickly in your experience?
Glyn in Dallas
Robin Melzer
So I just had this surgery Friday and I feel like it is sticking out further than it did before the surgery. Was this your experience in the beginning also??
Pat
Really scared for my boyfriend who is having this surgery very soon. I need to know what is the best way to help him..
tlaschinsky
Very informative and I see you have other posts, sorry yours came back. I am about 4 weeks post-op and yes, very similar experience. Rest is important and I wont’ lift anything over 10lbs until my 6 weeks is up and I have my follow-up appt. The hardest thing is to rest when you feel better! At 3 weeks and even today…I feel pretty good…so I tend to over do things. Not by lifting or house cleaning, but posture, the way I turn, walking too much etc. So keep that in mind and keep on resting.
I didn’t use ice as inflammation is good for healing so I let that just be. I also didn’t use the pain meds they prescribed but I did use high dose CBD oil which worked AMAZING! (Legal in my area.) Still looked swollen a few days ago but recently has flattened out.
Surprised by your photos, looks like you didn’t have any tape on your incision. I had to take mine off after 10 days…tip: go into bath or shower and let the warm water ‘melt’ the glue of the tape away then gently pull strips off one by one…slooooowwly! 🙂
I also found sleeping w/pillow on top felt good. Like a bit of weight for support but not uncomfortable weight. I’m a side sleeper but couldn’t sleep that way for a few weeks. I guess really, it’s about doing what is comfortable and everyone will be different.
Sneezing wasn’t as bad as I thought it would be but even now when I cough or sneeze I put my hands to my incision for extra support. A hernia support belt is good idea too. I wore that for the first while once things felt better and when I need extra support. I will wear it in the future too when I need to do any lifting to prevent re-occurence hopefully!
Josephine Adamo
I was just diagnosed with Umbilical and Inguinal hernias with a cyst in the Inguinal hernia.Im pretty scared right now because of it. Your story has helped me a lot thanks
Janet Brown
I am literally 30 hours out from umbilical hernia surgery done with out mesh and laparoscopically. I have to wear a tight velcro wrap for the next week until my post op visit. I had a tummy tuck in 1995 and a hernia was found and repaired. Took me a long time to find a comfortable sleeping position last night. I have been dealing abdominal pain for the last few years. It would come and go felt like I had been punched in my gut. Had all the various tests, upper scope, colonoscopy, celiac testing. All negative. On a whim I went to see a plastic surgeon for my aging neck and face consult and asked him to see if my 1995 procedure was still intact (it is!) he then said that I had the hernia. He palpated around my navel and surrounding areas and immediately produced the same pain I usually have which lasted for quite some time after. I have to wonder if the two are related? He also pulled up a CT scan I had done in August of 2018 ER visit due to abdominal pain and the separation of the facia was present then! No one caught it! So how awesome it would be if my symptoms are alleviated! Curious to know if anyone else may have experienced this?
Donna White
My op., 4 days ago, several small hernias, 10 centimeter mesh. Should have given me suppositories after the op, I swelled up like a balloon and was admitted back for another night.such a simple solution, dammit. Glycerin suppositories. A tip: to get out of bed, angle yourself flat at 90 degrees (rightangle) to the bed, slide forward slowly onto a solid hassock and the side of the bed acts as a lever. The hassock shouldn’t be too close to the top of the bedside, for better manoeuverability. It works for me, anyway. Busy looking up when I can lie on my side. I’m 66, so possibly a little less resilient than you are, but coping well right now. Thanks for your post x
Giovanna
Thank you for your honesty! I have had an umbilical hernia since my first child(who is now 3) and after my daughter(who is now 6months) my hernia got 10x worse. People are constantly asking how far along I am bc I have such a large bulge. And not to mention it’s painful. But I’m not going to lie, reading your experience made me even more nervous to have the surgery! My main concern is relying too much on anyone else to help. I mean I have a 6month old so I can’t picture not being able to pick her up for a whole week. I agree, every situation is different but I’m anxious about giving up my independence. But thanks again for your post and sharing your step by step recovery process and tips!
Cristal
Not a rubber, but definitely a go-go-go person. I’m 36hr post op, skipping the opiates cause I’m also 6weeks post partum, plus wrangling a hyper 4yo. Also finding this recovery to be much harder than anticipated. Your tips are helpful and the post overall reassuring. Looking forward to more relief in the coming days!
Nona
Thank you for this post! There still aren’t many personal accounts of hernia repair online, even three+ years later.
Melissa
2020 and these tips are still true. In 2012, while 34 weeks pregnant, I had my appendix and gall bladder removed. These tips are the same I would have given then. 6 weeks later, emergency c section: same tips. And January 2020 laparoscopic umbilical hernia repair with mesh: same tips. That pillow is also amazing to squeeze against your core when you cough or sneeze. Laughing hurt a lot!
Jason
Thank you so much for sharing this story. I had same surgery, umbilical hernia repair with mesh with classic cut open non laso. I would concur with all your details but my doc said 4 to 6 weeks before I can resume normal activity. I workout with kettlebells 5 days per week and do bench press on the 6th day. Being strong & active is my identity so its been hard for me. I’ve purchase some very small kettlebells (5 & 10 lbs) to slowly get back into shape. I was working with a 62 lbs. kettlebell before surgery. My big FEAR is that the mesh will get rejected by my body like in the late night tv adds from lawyers. But I was informed that my surgeon does 6 of these procedures a day and no issues.
Rebecca Jensen
Hi, it was great to read your story because slot of the things you did to help , I have done too. I’m on my 10th day of recovery and I still have a bit of pain and sometimes it radiates to one side and bending is hard. Also I noticed my belly button is pushed so far in and it’s hard to see which is strange to me. It’s been a very challenging not using your core muscles!
I’m hoping maybe in six or 8 weeks I’ll be able to get back into running. I hope everything healed for you! Have you had any problems or are you back to normal?